Teratomas grow teeth because they contain all three embryonic germ layers, and when the ectodermal component differentiates the way it would during normal fetal development, it can produce enamel, dentin, and even fully formed tooth-like structures. That is the short answer. The longer, more useful answer requires understanding what a teratoma actually is, why its biology is completely different from normal tooth development, and why those "growing teeth" you may have read about online are almost never actually forming new teeth over time inside the tumor.
Why Do Teratomas Grow Teeth, and Can They Grow Back?
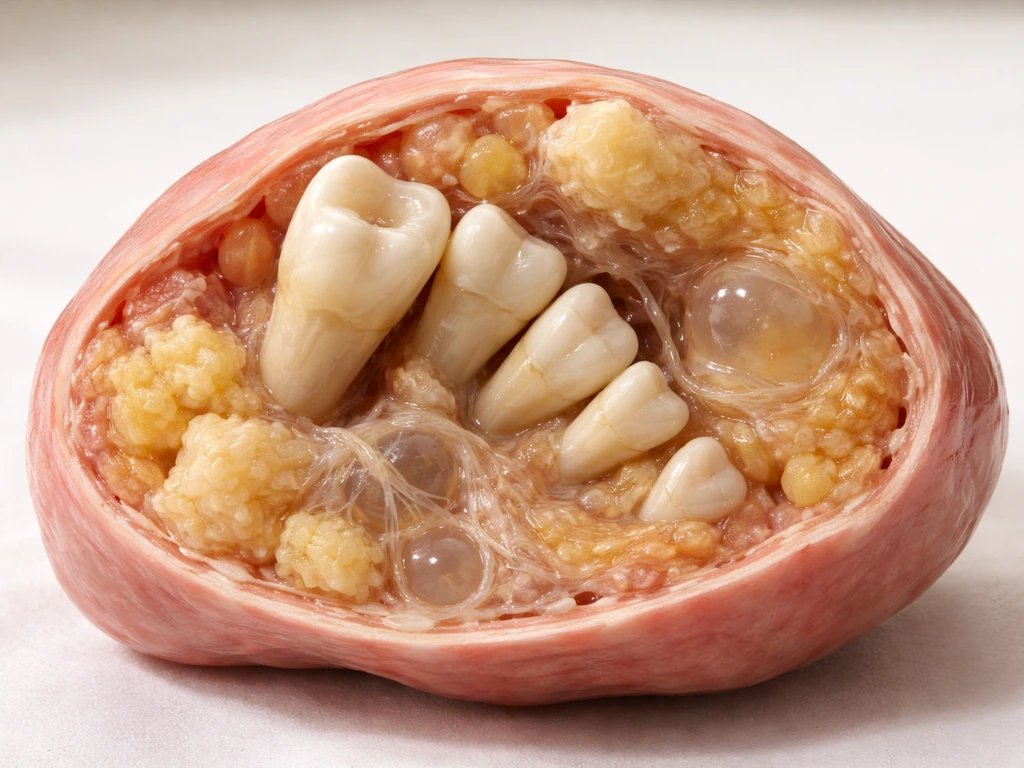
What a teratoma actually is (and where the teeth come from)

A teratoma is a type of germ cell tumor that contains tissue from more than one embryonic layer. We develop from three primary germ layers: ectoderm, mesoderm, and endoderm. Mature teratomas are composed of fully differentiated somatic tissues from all three of those layers, which is why a single tumor can contain skin, hair, fat, muscle, cartilage, thyroid tissue, gastrointestinal epithelium, and yes, teeth. Immature teratomas, by contrast, contain primitive embryonal-like tissue rather than well-organized adult-type structures, and they carry a much higher risk of malignant behavior.
The most common type by far is the mature cystic teratoma (sometimes called a dermoid cyst). In the ovary, roughly 99% of teratomas are composed of mature tissue and are clinically benign. Only about 1% are considered immature, and those are the ones with malignant potential. If you want a deeper dive into how ovaries can grow teeth through this exact mechanism, that context is worth reading. The teeth found in these tumors are not random accidents. They are the direct result of tissue that was always going to try to be teeth, given the right cellular environment.
How ectodermal tissue inside a teratoma actually makes enamel and dentin
Normal tooth development is a highly coordinated conversation between two tissue types: dental epithelium (ectodermal origin) and dental mesenchyme (neural crest-derived ectomesenchyme). Enamel is produced by ameloblasts, which come from the epithelial side. Dentin is produced by odontoblasts, which come from the mesenchymal side. These two cell populations signal back and forth using molecular pathways including Wnt, BMP, FGF, and Sonic Hedgehog (Shh). Neither tissue type can make a tooth on its own. They have to cooperate.
Inside a teratoma, that same cellular machinery can be present because both ectodermal epithelium and mesenchymal tissue are part of the tumor's composition. When these components happen to be organized in a way that mimics the reciprocal signaling of normal tooth development, they can produce structured dental tissue: enamel-forming ameloblast-like cells layered over dentin-producing odontoblast-like cells. This is not random chaos. It is misdirected but recognizable embryologic differentiation. The ectodermal epithelium within the tumor essentially does what ectodermal epithelium is programmed to do when it receives the right mesenchymal signals. The result can look, radiologically and histologically, remarkably like an actual tooth.
This is also why tumors can grow teeth in the first place. It is not magic or mutation in the conventional cancer sense. It is developmental programming running in the wrong place at the wrong time, using the same molecular signals that build real teeth in a developing jaw.
What controls the growth patterns inside these tumors
The same signaling pathways that control tooth development in normal embryology, primarily Wnt, BMP, FGF, and Shh, appear to govern how dental-like structures organize within a teratoma. Research has shown that overactivating Wnt/beta-catenin during tooth initiation upregulates Shh expression and drives the delimitation of odontogenic fields. In a teratoma, these pathways are not being orchestrated by a developing embryo. They are operating within a disorganized mass of mixed tissue types, which is why the resulting structures, while sometimes remarkably tooth-like, are not perfectly formed teeth in most cases.
The degree of organization matters clinically. Mature teratomas produce well-differentiated tissue with recognizable architecture. Immature teratomas contain primitive neuroectodermal tissue that has not completed differentiation, which is part of what makes them biologically aggressive. From a dental-tissue perspective, this distinction means that organized tooth-like structures (complete with pulp, dentin, and enamel) are more characteristic of mature teratomas, while immature ones are less likely to produce well-formed dental structures and more likely to cause serious medical problems.
Do teratomas actually keep growing new teeth over time?
This is the question most people actually want answered, and the honest answer is: almost certainly not in the way you are imagining. When people read that a teratoma "grows teeth," they often picture a tumor that is actively forming new teeth over time, the way a child's mouth produces new molars. That is not what happens. The tooth-like structures found in mature teratomas are almost always already-formed tissue that becomes visible or detectable as the tumor itself enlarges, not because new dental structures are being created.
Mature teratomas grow slowly. One imaging study found that small sonographically detected mature teratomas under 6 cm grew at an average of only about 1.8 mm per year in premenopausal women, and actually shrank by about 1.6 mm per year in postmenopausal patients. That is the overall tumor growing, not the dental components actively differentiating. A separate sellar teratoma case report explicitly framed mature lesions as not exhibiting the kind of rapid progression seen in actively malignant processes. The teeth are already there in the tissue. They are not being manufactured on an ongoing basis.
There is something called growing teratoma syndrome (GTS), which sounds alarming but refers to a specific clinical scenario: tumor markers normalize during treatment, yet the mass continues to enlarge, and histology confirms mature teratomatous elements in the growing portion. Even in GTS, the "growth" is the tumor mass expanding, not new dental organogenesis happening in real time. It is a clinically important distinction because GTS affects how surgeons approach re-intervention.
It is also worth noting that metachronous teratomas can develop: new, separate teratomas can arise in the same patient over time. So if someone has a teratoma removed and later develops another one with tooth-like structures, that is a new tumor, not the same one regrowing its teeth. This affects how clinicians interpret "recurrence" versus new disease.
What happens medically when a teratoma contains teeth
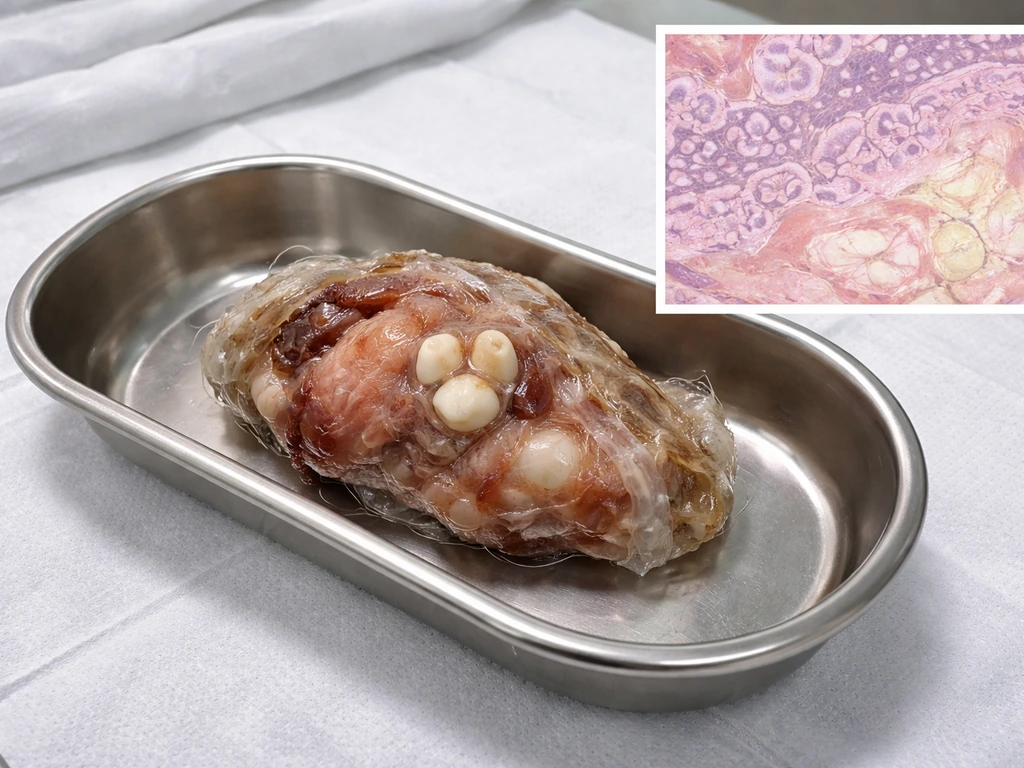
Finding tooth-like structures in a teratoma does not change the fundamental treatment approach, but it does confirm tissue maturity, which is clinically useful. The standard treatment for a symptomatic or enlarging mature teratoma is surgical removal, most commonly via laparoscopic cystectomy. Recurrence after complete resection is relatively low: reported surgical recurrence requiring re-intervention runs around 7.6% within 2 years after laparoscopic removal of a mature cystic teratoma. An entirely mature, completely excised teratoma should not recur. Recurrence is more of a concern when excision is incomplete or when immature elements are present.
Malignant transformation within a mature cystic teratoma is rare, reported at roughly 1 to 3% overall, but the risk increases with age and with tumor size above 10 cm. This is why postoperative follow-up matters even when everything looks benign at surgery. The goal is to catch any malignant transformation or new tumor development early, not to monitor ongoing dental tissue formation.
Imaging is central to evaluation. Ultrasound is typically the first-line tool, with CT and MRI used for more detailed characterization. Tooth-like calcifications on imaging are actually a useful diagnostic clue. If you or someone you know has been told there are calcifications or a "Rokitansky nodule" on an ovarian ultrasound, that is often a mature teratoma presenting in a classic way. Ask for a referral to a gynecologist or oncologist with experience in ovarian lesions. Watchful waiting may be appropriate for small, asymptomatic lesions, but the decision needs to be made with a clinician who knows your full picture.
How teratoma teeth are completely different from normal tooth development
Normal human tooth development follows a rigid, scheduled program. Primary (baby) teeth begin forming before birth and erupt in a predictable sequence starting around 8 to 12 months of age, with central incisors typically among the first. Permanent teeth follow their own timetable, with first molars and incisors erupting around age 6 to 8. Each tooth forms through a precise sequence of stages: initiation, morphogenesis, differentiation, and mineralization. That sequence requires the full embryological architecture of a developing jaw, complete with neural crest cell migration, signaling from surrounding tissues, and mechanical cues from the oral environment.
None of that infrastructure exists inside a teratoma. What a teratoma has is a disorganized but biologically active mix of tissue types that can partially replicate the epithelial-mesenchymal signaling environment. The result can be a recognizable dental structure, but it is not a tooth in the functional sense. It cannot erupt. It is not anchored in a periodontal ligament. It does not respond to bite forces. It is more analogous to an odontoma, a benign developmental anomaly that produces organized dental tissue outside of normal jaw architecture.
This also connects to why human teeth do not regenerate after they are lost. There is no adult stem cell population in the human mouth that can restart the full tooth-development sequence from scratch. Once the enamel epithelium sheds after eruption (a process called apoptosis of the enamel organ), the tissue capable of making enamel is gone. The question of whether stem cells can grow teeth is being actively researched, but we are not there yet clinically. Teratoma teeth are not an example of regeneration. They are an example of misdirected embryologic development that happened to produce dental tissue in the wrong location.
It is also worth distinguishing teratomas from other lesions that can harbor calcified or tooth-like material. Cysts that grow teeth represent a separate category of odontogenic lesions with different developmental origins and clinical behaviors. And bony outgrowths in the mouth like mandibular tori, which can sometimes alarm patients, are an entirely different phenomenon with no dental tissue formation involved at all.
The myths worth clearing up right now
The internet has done a spectacular job of making teratoma teeth sound like science fiction, and some of the myths floating around are genuinely misleading. Here are the ones that come up most often, with direct corrections.
- Myth: A teratoma is a "twin" growing inside you with its own developing teeth. Reality: Teratomas are germ cell tumors. They are not vestigial twins. They arise from pluripotent germ cells, not from a separate fertilized egg. The teeth they contain are not the teeth of a separate person.
- Myth: The teeth inside a teratoma keep growing and multiplying over time. Reality: Mature teratomas grow slowly as masses. The dental structures within them are essentially already-formed tissue. New tooth organogenesis is not occurring inside an established mature teratoma.
- Myth: Teratoma teeth prove humans can regenerate teeth. Reality: They prove the opposite. Teratoma teeth form through misdirected embryologic programming, not through any regenerative capacity of adult tissue. Normal adult human teeth cannot regrow after loss.
- Myth: All teratomas containing teeth are cancerous or dangerous. Reality: Mature teratomas with dental structures are almost always benign. The presence of teeth-like structures is actually associated with mature, well-differentiated tissue, which is a good sign clinically. Malignant transformation is possible but rare.
- Myth: Removing the teratoma means removing something that will just grow back with new teeth. Reality: Complete surgical excision of a mature teratoma is curative in the vast majority of cases. The long-term recurrence rate after surgical excision is approximately 4.2%, and that recurrence is the tumor mass, not the dental tissue specifically regenerating.
What to do if you suspect or have been diagnosed with a teratoma

If imaging has revealed a mass with calcifications or tooth-like structures, especially in the ovary or pelvis, the most important thing you can do is get a proper evaluation with a specialist rather than waiting to see what happens. Most mature teratomas are benign, but the only way to confirm maturity is through pathology after excision or biopsy. Do not rely on the presence of teeth-like structures on imaging alone to conclude the lesion is benign.
Here is what a typical evaluation pathway looks like for a suspected ovarian teratoma:
- Pelvic ultrasound to characterize the lesion (size, cystic vs. solid components, calcifications).
- Serum tumor markers (CA-125, AFP, hCG, LDH) to help distinguish mature from immature or malignant disease.
- CT or MRI for further characterization if ultrasound findings are ambiguous or the mass is large.
- Referral to a gynecologic oncologist if the lesion is over 10 cm, if tumor markers are elevated, or if the imaging suggests mixed or solid components.
- Surgical resection (typically laparoscopic cystectomy) with pathologic examination of the entire specimen.
- Postoperative follow-up at intervals determined by your surgeon, with attention to symptoms and recurrence risk.
Do not let the word "teratoma" or the presence of tooth-like structures panic you, but also do not let the fact that most are benign lead you to delay evaluation. Size, age, and histology all matter. A 4 cm asymptomatic lesion in a 25-year-old is a very different clinical conversation than a 12 cm mass in a postmenopausal patient. Get the evaluation, ask your doctor specifically about the maturity of the lesion and the surveillance plan, and make sure follow-up imaging is scheduled.
The teeth inside a teratoma are genuinely one of biology's more striking examples of what happens when developmental programming goes off-script. They are real dental tissue, formed by the same molecular machinery that builds teeth in a jaw, but they are not evidence of regeneration, they are not a twin, and they are not actively multiplying. They are a fascinating, sometimes dramatic, but ultimately manageable finding when caught and treated appropriately.
FAQ
If imaging shows teeth in a teratoma, do the teeth continue to form as the tumor gets bigger?
Usually, they do not. The tooth-like material in mature teratomas is typically already differentiated tissue that becomes more apparent as the cyst enlarges. If you are seeing new calcifications or obvious “growth” on serial scans, that more often reflects expansion of the overall lesion or change in imaging appearance, not ongoing formation of brand-new enamel and dentin units.
Can doctors tell for sure whether a teratoma is mature just from seeing teeth or calcifications on ultrasound or CT?
Imaging alone cannot reliably confirm maturity. Calcifications and tooth-like structures strongly suggest a mature cystic teratoma, but definitive maturity (and whether any immature or malignant components are present) requires tissue evaluation after biopsy or surgical excision. This is why clinicians emphasize pathology over appearance.
When would a clinician choose monitoring instead of surgery for a mature teratoma with teeth?
If the mass is small and you have no concerning symptoms, some clinicians may consider watchful waiting, but the decision hinges on factors like size, growth rate, your age, and ultrasound features. Even then, follow-up imaging is usually scheduled on a defined timeline, because incomplete excision or a missed immature component can change management.
If teeth appear again after surgery, does that always mean the original teratoma regrew?
Metachronous teratomas mean you can develop a new, separate tumor later, so “recurrence” may actually be new disease. This matters for follow-up because management and counseling differ when pathology suggests a new primary lesion rather than residual tissue from the original surgery.
What exactly is growing teratoma syndrome, and does it imply new teeth are forming inside the tumor?
Growing Teratoma Syndrome is uncommon but it is specific: tumor markers decrease or normalize after treatment while the mass enlarges, and pathology shows mature tissue in the enlarging portion. It does not mean new tooth organogenesis is occurring; it means the tumor is expanding with mature elements despite systemic marker response.
Do teratoma teeth cause tooth-like symptoms such as eruption or biting sensitivity?
Not in the functional, eruptive sense. Teratoma dental tissue lacks the normal supporting structures, so it cannot erupt, bite, or respond to chewing the way real teeth do. If a patient is having pain or pressure, that symptom usually comes from mass effect, inflammation, or complications rather than tooth “activity.”
Can teratomas with teeth cause sudden symptoms, like severe pain, and why?
Sometimes. Teratoma can rupture or leak contents, which may trigger inflammation and acute pain, and occasionally there can be torsion in ovarian cases. Those events do not indicate new dental growth, but they do make urgent evaluation important because they can change urgency and treatment approach.
Does having teeth in a teratoma increase the chance it becomes cancer?
Yes, but typically it is not based solely on the presence of teeth. The risk of malignancy is higher with immature components, larger tumor size (notably beyond about 10 cm), and increasing age. If any concerning features are present, clinicians may recommend earlier surgery and closer postoperative surveillance.
After complete excision, what follow-up schedule is usually recommended, and what does it depend on?
For ovarian mature cystic teratomas, complete removal generally has a low recurrence rate, but your follow-up plan depends on whether resection was complete and what pathology showed. Ask your clinician about how soon and how often you should have repeat imaging, because surveillance strategy differs by age, tumor size, and whether there were immature elements.
If a report mentions calcifications or “tooth-like” findings, how do doctors know whether it is actually a teratoma versus another lesion?
If imaging shows tooth-like material, it is essential to consider other diagnoses such as odontogenic lesions in the jaw, and benign bony outgrowths like tori. The key practical point is anatomic location and tissue type: ovarian or pelvic “teeth” usually point toward teratoma, while mouth lesions with calcifications may require a different workup pathway.
Learn if cysts can grow teeth or hair-like tissue, how jaw cysts are diagnosed, and when to get urgent care.
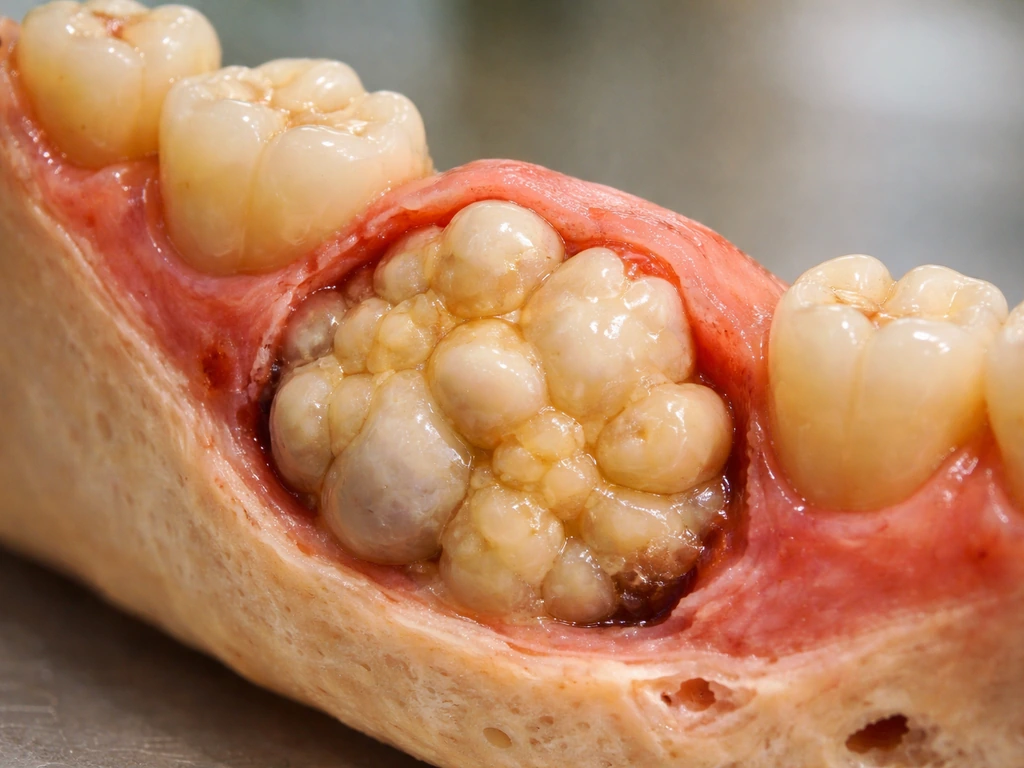
Can a tumor grow teeth or tooth-like tissue? Learn the rare types, why it happens, red flags, and next steps.

Why humans have only baby and permanent teeth: eruption timeline, limits of enamel regrowth, and common exceptions to kn

