You cannot make wisdom teeth grow in straight at home. The direction and angle a wisdom tooth erupts is determined almost entirely by the anatomy you were born with: the size of your jaw, the space available behind your second molars, and the position the tooth bud formed in years before eruption even began. No exercise, diet, massage, or supplement changes any of that. What you can do is keep your gum tissue healthy to reduce the chances of complications, monitor symptoms carefully, and work with a dentist or oral surgeon to decide whether watching and waiting, orthodontic mechanics, or extraction is the right call for your specific situation.
How to Make Wisdom Teeth Grow Straight: What Actually Works
What actually determines whether wisdom teeth come in straight
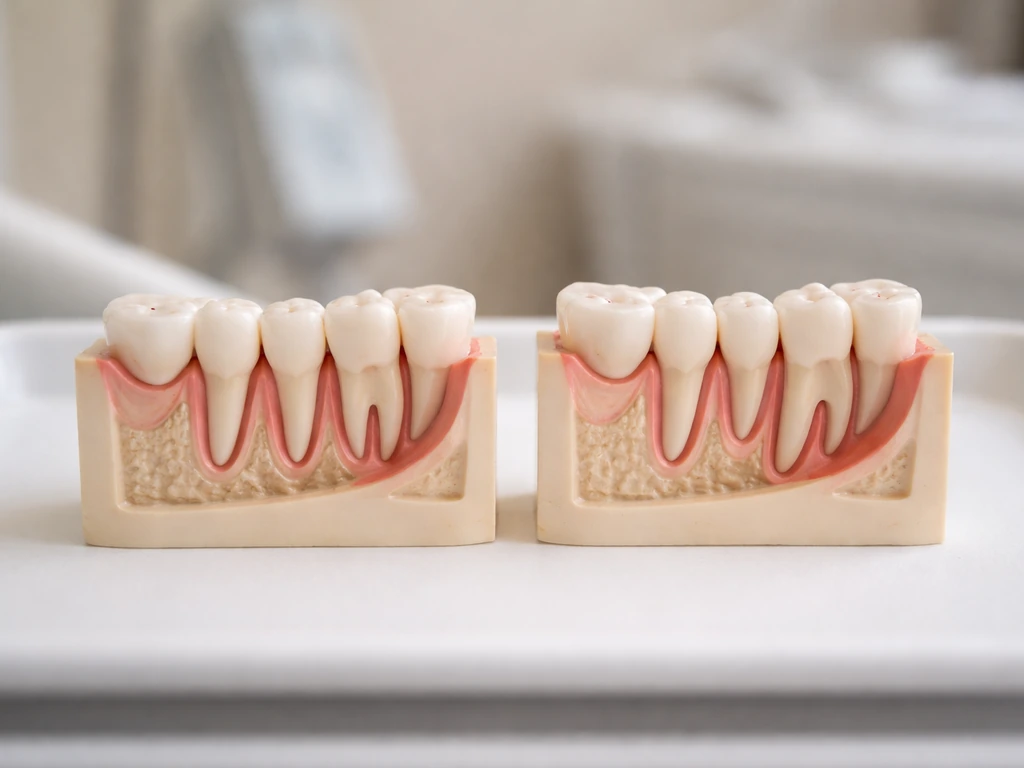
Three things control eruption direction, and none of them are under your influence once you are past early childhood. First is jaw size: if your jaw does not have enough space behind the second molar, the erupting third molar physically has nowhere to go except sideways, forward, or deeper into the bone. Second is the tooth's angulation in the bone, which is set by where the tooth bud developed. Third is the relationship between the tooth and the anterior border of the ramus (the vertical part of the lower jaw), which is why dentists use classification systems like Pell and Gregory to describe just how much the tooth is physically blocked by bone.
This matters because a lot of internet advice implies that if you just eat the right foods or do jaw stretches, the tooth will "find its way." That is not how eruption works. The eruptive pathway is a mechanical process driven by root development pushing the crown upward and forward. If the crown is angled toward the neighboring tooth or buried under bone, root growth is not going to straighten it out. It is the equivalent of growing a plant in a container that is too small: the roots will grow, but the plant cannot grow straight because the structure around it does not allow it.
It is also worth being clear about something that fits directly into the focus of this site: human teeth do not regenerate or reform to correct their own position. Once a wisdom tooth is partially erupted at an angle, it will not spontaneously straighten itself over time. The crown shape, root orientation, and eruption angle are fixed. Understanding this biological reality is the starting point for making a smart decision about what to do next. This includes understanding what you can and cannot do at home if your goal is making teeth appear longer naturally.
Wisdom tooth eruption timeline and what goes wrong
Wisdom teeth (third molars) typically begin erupting between ages 17 and 25, though the MSD Manual notes the range broadly as 17 to 21 years for initial eruption, with some people not seeing movement until their mid-twenties. By your late twenties, if a wisdom tooth has not erupted, it is unlikely to do so on its own without complications. Some people never develop them at all.
When things go wrong, the pattern of misalignment follows predictable categories. Dentists use Winter's classification to describe the angulation of an impacted wisdom tooth relative to the second molar next to it. The main types are:
- Vertical: the tooth is upright but still stuck, most commonly due to lack of space. This is actually the most frequently seen angulation pattern in studies.
- Mesioangular: the tooth is tilted forward (toward the front of the mouth), angling into the second molar. This is one of the more common types and a frequent cause of pain and damage to the neighboring tooth.
- Distoangular: the tooth tips backward, toward the back of the jaw. Often harder to extract if removal becomes necessary.
- Horizontal: the tooth lies almost completely on its side. This pattern is predominantly seen in the lower jaw and is almost always impacted.
Partial eruption, where the tooth breaks through the gum but does not fully emerge, is a particularly common setup for problems. The flap of gum tissue covering a partially erupted tooth (called the operculum) creates a pocket where bacteria collect and brushing cannot reach. This is the direct cause of pericoronitis, an inflammatory and often infectious process in the gum tissue around the erupting tooth.
What you can realistically do at home (and what is just internet folklore)

The myths worth addressing directly
You will find advice online suggesting that chewing hard foods, massaging your gums, taking specific vitamins, or using essential oils can guide wisdom teeth into proper alignment. None of these have any biological mechanism behind them. Chewing does not reposition a tooth that is angled against bone or a neighboring root. Gum massage does not affect the direction a tooth bud is oriented in your jaw. Vitamins support general bone health but cannot reshape an eruptive pathway that is already anatomically constrained. These ideas get spread because people want there to be a home remedy, but the anatomy simply does not work that way.
Similarly, some people believe that if they had their other teeth straightened with braces or aligners as a teenager, their wisdom teeth will now have room to come in straight. Sometimes this is true for space availability, but braces do not change the angulation of a tooth bud that is already positioned horizontally or mesioangularly in the bone.
What genuinely helps
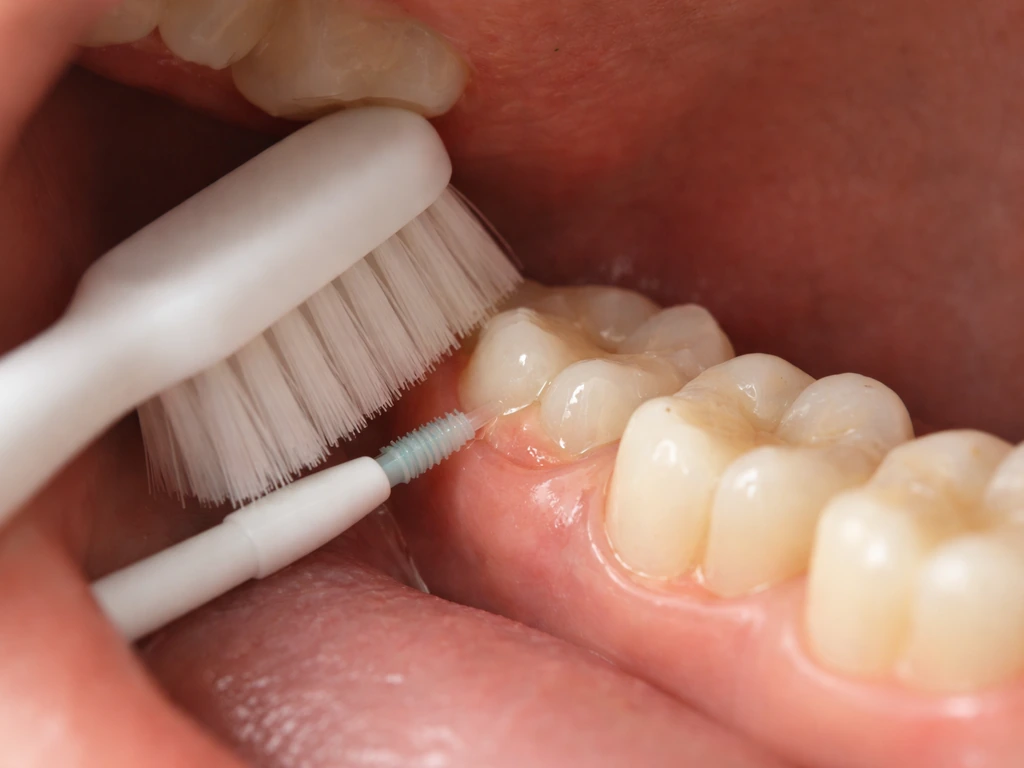
While you cannot change the eruption direction, you can meaningfully reduce the risk of complications during the eruption process. While you cannot make a tooth grow faster, you can still work with a dentist to manage risk and decide whether monitoring, orthodontic options, or extraction is appropriate cannot change the eruption direction. Clinical evidence supports a few specific measures for people whose wisdom teeth are erupting or partially erupted:
- Thorough brushing around the erupting tooth: use a soft-bristle toothbrush and angle it toward the back of the mouth to reach as far behind the second molar as possible.
- Interdental cleaning: using small interdental brushes or floss around the area reduces bacterial load in the gingival pocket.
- Chlorhexidine mouthwash: rinsing with a chlorhexidine-based mouthwash has clinical evidence supporting its ability to reduce pericoronitis symptoms related to erupting wisdom teeth.
- Salt water rinses: a warm saline rinse several times a day can reduce inflammation and keep the area clean, particularly if gum tissue is tender.
- Avoiding trauma to the area: biting hard foods directly on the erupting tooth can aggravate already inflamed gum tissue.
These steps do not make the tooth grow straight. In other words, wisdom teeth generally cannot grow longer or reach a better position just because time passes. They keep the tissue environment healthy enough to reduce infection risk while the tooth is doing whatever it is anatomically going to do, and while you figure out the right treatment path.
When dental or orthodontic treatment is the actual answer
For most misaligned or impacted wisdom teeth, the realistic options involve a dentist or oral surgeon rather than anything you do at home. If you are asking how to make molars grow in faster, the key point is that eruption timing and direction are mostly determined by your anatomy, not at-home steps. The treatment path depends heavily on the angle and depth of impaction, your age, and whether symptoms or pathology are present.
Orthodontic eruption guidance (using brackets and traction to pull an impacted tooth into position) is occasionally used for wisdom teeth, but it is far more commonly applied to canines and premolars. Canine teeth growth length is also something a dentist can evaluate with the right exam and guidance, since it depends on anatomy and eruption patterns rather than home techniques more commonly applied to canines and premolars. Wisdom teeth are rarely candidates because of their position, root morphology, and the limited functional value of guiding them versus simply removing them. If a dentist or orthodontist thinks traction is worth attempting in your specific case, they will tell you after reviewing imaging.
For the majority of people with a symptomatic or pathologically positioned wisdom tooth, extraction is the most evidence-based resolution. NICE guidelines identify specific indications for extraction, including unrestorable decay, non-treatable pulpal pathology, recurrent pericoronitis, cellulitis or abscess, and cysts or tumors associated with the follicle. Critically, the NICE guidance also notes that a first episode of pericoronitis, unless particularly severe, is not on its own an automatic indication for surgery. This means your first painful episode may be managed conservatively while you and your dentist decide on a longer-term plan.
For asymptomatic impacted wisdom teeth, the evidence is genuinely mixed. A Cochrane review found insufficient evidence to support or refute routine prophylactic removal of asymptomatic impacted wisdom teeth in adults. The American Association of Oral and Maxillofacial Surgeons (AAOMS) provides its own evidence-based parameters for management, and the recommendation often comes down to the patient's specific risk profile, age, and imaging findings rather than a blanket rule. Younger patients (late teens to early twenties) generally recover faster from surgery and face lower risk of complications, which factors into timing decisions.
How to manage pain and prevent problems while you wait
If your wisdom tooth is erupting and causing discomfort but you are not yet at the point of treatment, the following evidence-aligned steps help reduce symptoms and prevent escalation:
- Take over-the-counter pain relief as directed: ibuprofen (if not contraindicated) works better than acetaminophen alone for dental inflammation because it addresses the inflammatory component, not just the pain signal.
- Rinse with warm salt water or chlorhexidine mouthwash after meals and before bed to keep bacteria out of the gum pocket.
- Brush gently but thoroughly around the area. Skipping brushing because it hurts makes the infection risk significantly worse.
- Avoid smoking: smokers have dramatically higher rates of pericoronitis and post-surgical complications.
- Watch for warning signs that need prompt dental attention (see below).
Warning signs that mean see a dentist now, not later
Pericoronitis affects roughly 1 in 20 people with erupting wisdom teeth, and almost all cases (about 95%) involve the lower third molar. Most resolve with local treatment, but some escalate. Contact a dentist promptly if you notice any of the following:
- Swelling spreading beyond the immediate gum area, especially toward the cheek, jaw, or throat
- Difficulty opening your mouth (trismus)
- Pain that is worsening rather than improving after 2 to 3 days of home care
- Fever, swollen lymph nodes in the neck, or general malaise alongside tooth pain
- Visible pus or discharge from the gum tissue
- Difficulty swallowing
Evidence-based pericoronitis management prioritizes local treatment and oral hygiene rather than antibiotics as a first step. Systemic antibiotics are reserved for cases where there is evidence of spreading infection or systemic involvement. Do not expect or ask for antibiotics at a first mild episode; local treatment and dental evaluation are the appropriate response.
X-rays, diagnostics, and how to actually decide what to do
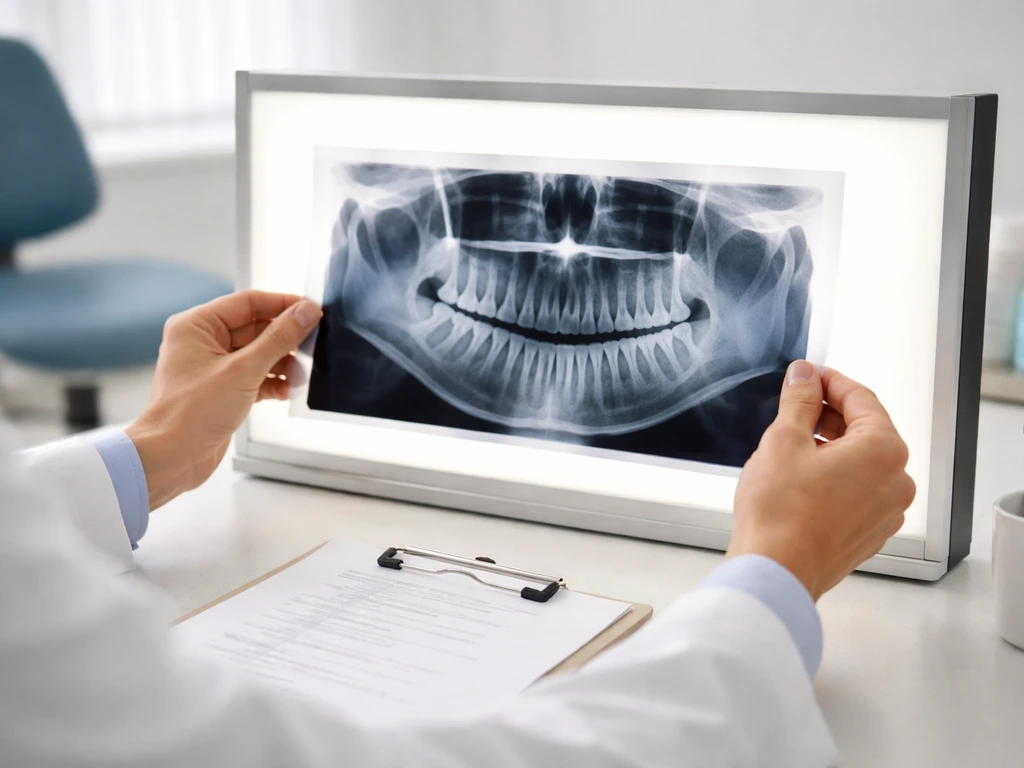
No one can tell you what your wisdom teeth are doing based on symptoms alone. The only way to know the angulation, depth, root development, and relationship to adjacent structures is imaging. A panoramic X-ray (OPG) gives a broad view of all four third molars at once and is usually the starting point. For more complex cases, a cone beam CT (CBCT) scan provides a three-dimensional picture that shows the tooth's exact relationship to the inferior alveolar nerve in the lower jaw, which is a critical factor in surgical planning.
When a dentist reviews your X-rays, they are assessing the angulation pattern (using Winter's classification), the depth and bone coverage (Pell and Gregory classification), root formation stage, and whether there is any evidence of adjacent tooth damage, cyst formation, or bone changes. This is not something to guess at based on pain location or how the gum feels.
Based on what imaging shows and your symptom history, here is a practical framework for deciding your next step:
| Your situation | What the evidence supports |
|---|---|
| No symptoms, wisdom teeth partially or fully impacted | Active monitoring with periodic X-rays; discuss risk profile with dentist or oral surgeon. Routine prophylactic removal is not universally recommended but may be advised based on your anatomy and age. |
| Mild gum pain or pressure, no swelling or fever | Improve oral hygiene, use chlorhexidine rinse, take OTC pain relief, and book a dental appointment within 1 to 2 weeks for imaging. |
| Recurring pericoronitis episodes | Get imaging and have a frank conversation about extraction. Recurrent episodes are one of the cleaner indications for removal. |
| Swelling, fever, difficulty opening mouth or swallowing | This is urgent. Go to a dentist or emergency dental service today. Spreading infection requires prompt professional management. |
| Confirmed impaction, deciding on timing of surgery | Younger patients (17 to 25) generally recover faster and face fewer complications. Discuss timing with an oral surgeon. |
If you are reading this alongside questions about speeding up eruption of other teeth or helping molars come in faster, the same core principle applies: eruption speed and direction are biologically driven processes with real anatomical limits. What changes between tooth types is how often intervention (braces, surgical exposure, extraction) is worthwhile versus simply monitoring. Wisdom teeth specifically have a lower threshold for extraction relative to other teeth because their functional value is limited and the risks of keeping a problematic one tend to outweigh the benefits.
The most useful thing you can do today is book a dental appointment if you have not had imaging done recently, keep the area as clean as possible in the meantime, and stop expecting a home remedy to change what is fundamentally an anatomical situation. If you are specifically searching for ways to make your teeth grow in, the key takeaway is that you cannot force wisdom teeth to straighten themselves at home. Once you have your X-rays in hand, the decision about monitoring versus treatment becomes much clearer, and you are making it based on actual information rather than guesswork.
FAQ
Can I make my wisdom teeth grow in straight with exercises, massage, or a special diet?
Not safely. Once a wisdom tooth is angled or partially blocked by bone, you cannot “train” it to straighten at home. The practical question is whether your tooth is likely to cause problems during eruption, which requires imaging and a symptom history, then a plan for monitoring, conservative care, or extraction.
If I got braces before, will that make my wisdom teeth come in straight?
Braces or aligners can sometimes help with spacing for other teeth, but they do not change the orientation of a wisdom tooth bud already positioned in the jaw. If your wisdom tooth is horizontally or mesioangularly impacted, orthodontics typically cannot overcome that built-in angulation, though it may be part of a broader plan to manage overall arch space.
What should I do if my wisdom tooth is only partially erupted and hurts?
If a wisdom tooth is partially erupted, you should treat it like an infection-risk site. Avoid aggressive probing or “digging” at the operculum, and focus on gentle cleaning plus the specific local measures your dentist recommends. If swelling, fever, worsening pain, or trouble swallowing develops, that is a reason to seek urgent evaluation rather than waiting.
How can I tell whether my wisdom tooth is truly impacted versus just erupting normally?
Pain alone does not tell you how impacted the tooth is or whether it is damaging nearby structures. Dentists base direction and depth on X-rays, and sometimes CBCT for nerve proximity. If you can only choose one step, schedule the imaging and evaluation rather than experimenting with home remedies.
Does one episode of pericoronitis always mean I need to get my wisdom teeth removed?
A first bout of pericoronitis does not automatically mean you need immediate surgery, but it does mean you should get evaluated promptly. Your dentist will decide whether to manage conservatively now and watch, or plan treatment based on severity, recurrence, and imaging findings.
Should I ask for antibiotics if my wisdom tooth gum is infected or inflamed?
Antibiotics are not the first-line fix for most mild cases because the core problem is often localized inflammation and bacterial buildup under the operculum. Antibiotics are generally reserved for cases with spreading infection signs or systemic involvement. Ask your clinician what they see clinically and on imaging before expecting antibiotics.
Do I always need a CBCT scan, or is an OPG X-ray enough for wisdom tooth planning?
Yes. For lower third molars, the key surgical risk is the relationship to the inferior alveolar nerve. If the nerve is close or overlapping, a cone beam CT may change the risk estimate and the surgical approach compared with a panoramic X-ray alone.
If my wisdom teeth haven’t erupted by my late 20s, should I ignore it?
“Not yet showing up by late 20s” can still be normal, but it also reduces the chance of spontaneous eruption without issues. If you suspect symptoms or crowding, you still need an exam and imaging because non-eruption can be due to impaction or lack of space, and the management decision depends on those findings.
Will my misaligned wisdom tooth fix itself if I wait longer?
Do not assume your wisdom tooth will straighten after time. Many angled wisdom teeth stay angled, and partially erupted ones can repeatedly inflame. The decision is based on imaging and risk factors like recurring pericoronitis, cysts, decay risk on the second molar, or bone changes.
What exactly does the dentist look for on the X-rays when deciding what to do with wisdom teeth?
Expect the dentist to evaluate more than “how it looks.” They usually consider angulation (like Winter’s), depth and bone coverage (like Pell and Gregory), root development stage, and whether there is contact or risk to the second molar, plus cyst or bone changes if present. Bring your symptom timeline to help interpret what you see on imaging.
Learn what can regrow in teeth, why enamel won’t, and safe options for missing, broken, or delayed eruption.
Myths vs reality on making a tooth grow faster, eruption timelines, safe habits, and dentist options for teens and adult
Know what can and cannot speed tooth eruption, movement, or regrowth, with age timelines and safe next steps.

