No, teeth do not grow back after grinding. Once enamel or dentin is removed by bruxism, attrition, or a dental procedure like tooth contouring or crown prep, that hard tissue is gone permanently. Your body has no biological mechanism to rebuild it from scratch. In short, why teeth don't grow back is because mature enamel and its enamel-forming cells are gone, and the body can only remineralize very early surface damage. The cells that formed your enamel (ameloblasts) disappear after your teeth erupt, so there is nothing left to restart the process. What CAN happen is limited: early surface-level enamel damage can be partially patched through remineralization with fluoride, and dentin has some capacity to lay down new material in response to injury. But if you are asking whether a noticeably ground-down tooth will fill itself back in, the honest answer is no.
Do Teeth Grow Back After Grinding? What to Expect
No, teeth don't grow back after grinding, here's the biology
This is one of the most persistent misconceptions in dental health. People notice their teeth feel different after grinding, or they see a dentist grind down a tooth during a procedure, and they wonder if the body will quietly fix it overnight. It won't. Mature dental enamel is acellular, meaning it contains no living cells once it has fully formed. The ameloblasts that built your enamel during tooth development are completely gone by the time your permanent teeth erupt. There is literally no cellular machinery remaining inside enamel to carry out any repair. This is fundamentally different from bone, skin, or even dentin, all of which retain some capacity for ongoing cellular activity and self-repair.
Scientific reviews confirm this clearly: mature enamel cannot regenerate itself after substantial mineral loss. Any research you see about 'enamel regeneration' is describing experimental, lab-stage approaches using biomimetic proteins or cell-based tissue engineering. None of these are available clinical treatments as of today. When a dentist or toothpaste ad talks about 'restoring enamel,' they mean remineralization of microscopic surface damage, not rebuilding enamel that has been physically removed.
What grinding actually removes (and why it matters)
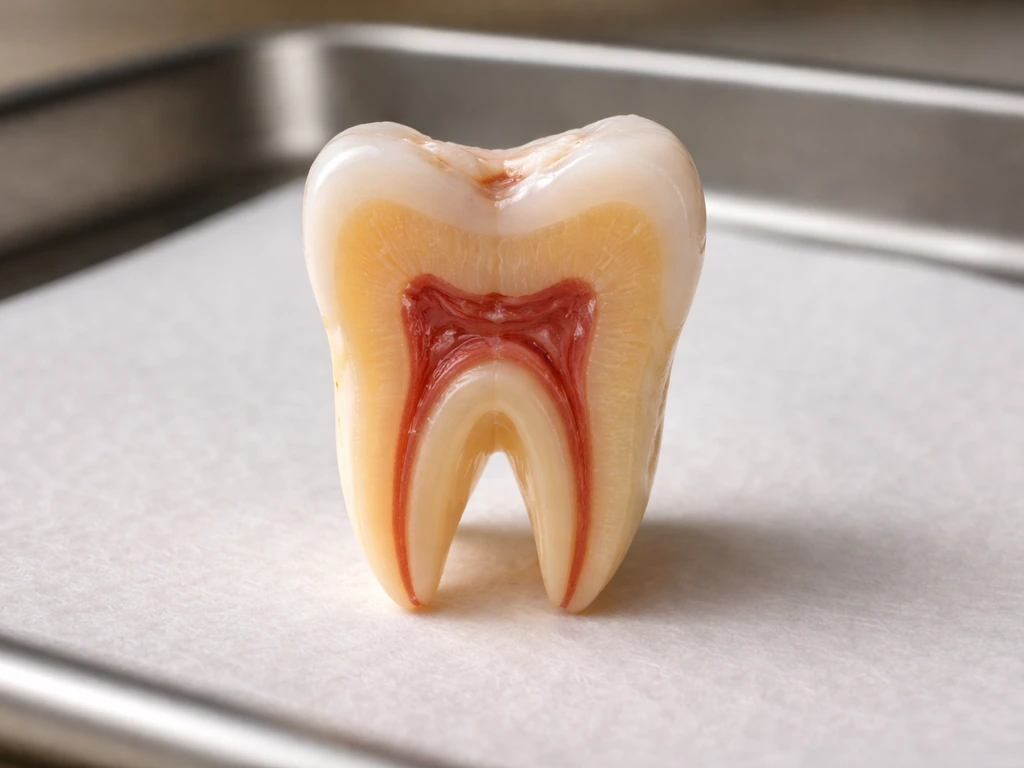
Understanding what 'grinding' removes helps you understand what you are working with. Teeth have three main hard tissue layers, and grinding can affect each one differently depending on how much pressure, how long it has been happening, and whether a dental procedure was involved.
| Layer | What it does | Can it repair itself? | What removal feels like |
|---|---|---|---|
| Enamel | Outer protective shell; no nerves inside | No (acellular; ameloblasts gone after eruption) | Often painless at first, but increases sensitivity over time |
| Dentin | Softer layer beneath enamel; contains tubules connected to nerve | Partially (odontoblasts can deposit tertiary dentin) | Sensitivity to temperature, sweets, and pressure |
| Pulp/nerve | Living tissue at the core; blood vessels and nerves | Limited (pulp capping can promote reparative dentin) | Pain, throbbing, or complete nerve death if severely damaged |
In chronic nighttime grinding (bruxism), enamel wears down gradually over months and years. In dental procedures, the removal is more precise but immediate: tooth contouring (enameloplasty) removes small amounts of enamel to reshape a tooth, while crown preparation can reduce the occlusal surface by roughly 1.5 to 2.0 mm, removing both enamel and sometimes dentin. The key point: enamel has no nerves, so early grinding damage often goes unnoticed until the dentin beneath becomes exposed.
What can actually repair itself (and what cannot)
Remineralization: the limited good news
Here is where there is a genuine but very limited bright spot. If grinding has caused only microscopic, surface-level enamel erosion and no physical chunks have been removed, remineralization can partially shore up that surface. Fluoride works by promoting the formation of fluorapatite, a more acid-resistant mineral, and this process can reverse very early demineralization. Over-the-counter fluoride toothpastes contain roughly 1,000 to 1,500 ppm fluoride, while prescription-strength options reach 5,000 ppm for more significant needs. This is real and useful, but it is not the same as regrowing enamel. Think of it like patching micro-cracks in a wall versus rebuilding the wall itself. Once enamel has been physically worn or ground away in measurable amounts, remineralization cannot fill that gap. Once you are seeing a noticeable gap or worn-down areas, it does not regrow, so the timeline is typically about protecting what remains and treating the surface how long does it take for enamel to grow back.
Dentin's limited self-repair ability
Dentin is a different story. Unlike enamel, dentin retains living cells called odontoblasts throughout your life, and these cells can respond to injury. With less severe damage, existing odontoblasts deposit what is called reactionary dentin. With more intense injury (when original odontoblasts are destroyed), new odontoblast-like cells can differentiate and produce reparative dentin. This is actually meaningful: it is why some teeth that have been ground or drilled close to the pulp do not immediately die. The pulp is fighting back by walling itself off. However, this process has limits. It takes time, it is not guaranteed, and it depends heavily on how close the grinding got to the pulp and how much tissue was affected. If the pulp is directly exposed, the situation becomes urgent and requires clinical intervention.
The pulp and nerve: where things get serious
If grinding has reached the pulp, the nerve tissue inside becomes disrupted and disorganized, and hypersensitivity spikes. The pulp can sometimes heal through reparative dentin formation, especially if the exposure is small and mechanical (rather than from decay). This is the basis for a dental procedure called direct pulp capping, where a protective material is placed over the exposed pulp to encourage healing. But outcomes depend on the size of the exposure, the condition of the tissue, and how quickly treatment happens. Left untreated, an exposed pulp typically does not self-heal into a healthy state. Because the nerves inside the tooth do not reliably grow back after this kind of grinding damage, left untreated it can progress toward infection does not self-heal into a healthy state. It progresses toward infection.
How to tell how serious your situation is
The symptoms you are experiencing right now are your best guide to how deep the damage goes. Use these as a rough roadmap:
- No sensitivity at all after minor contouring or smoothing: likely only enamel was touched. Monitor and maintain good fluoride hygiene.
- Mild sensitivity to cold drinks or sweets that passes quickly: dentin is probably exposed but not severely. Not an emergency, but worth a dentist visit soon.
- Sharp pain when biting, chewing, or tapping the tooth: this can indicate a crack or significant dentin/pulp involvement. Do not wait on this one.
- Lingering pain after temperature exposure (the tooth aches for 30+ seconds after a cold drink): this pattern suggests pulp involvement and needs urgent evaluation.
- Spontaneous throbbing pain with no trigger: likely pulp inflammation or the beginning of infection. This is a dental emergency.
- Visible chips, divots, or a noticeably shorter tooth: structural loss has occurred. Remineralization will not fix this. You need a dentist to assess restoration options.
- Swelling, gum tenderness around the tooth, or a bad taste: possible abscess. Seek care the same day.
Cracked teeth from grinding can be especially deceptive because they cause intermittent sensitivity to temperature and sweets, and sharp pain when biting, before the crack progresses into something worse. An untreated crack can eventually lead to a tooth abscess. If you had a dental procedure that involved grinding and now have worsening pain rather than improving comfort, that is not normal healing and needs to be checked.
What to do right now: self-care and when to see a dentist

Things you can do today at home
- Switch to a soft-bristled toothbrush and use gentle pressure. Aggressive brushing on already-thinned enamel or exposed dentin accelerates damage.
- Use a fluoride toothpaste twice daily. For extra support, your dentist can prescribe 5,000 ppm prescription fluoride if over-the-counter strength is not cutting it.
- If you have sensitivity, use a desensitizing toothpaste with potassium nitrate or stannous fluoride. These work by either calming the nerve signals (potassium nitrate) or physically occluding the dentinal tubules that transmit sensitivity (stannous fluoride). Use it consistently for a few weeks before judging the result.
- Avoid acidic food and drinks for now: citrus, soda, vinegar-based foods, and wine all soften enamel further. If you do consume them, rinse with water and wait 30 minutes before brushing.
- Use a straw for hot or cold drinks to reduce direct contact with sensitive surfaces.
- Do not grind further. If this damage came from nighttime bruxism, wearing a night guard is non-negotiable. A store-bought boil-and-bite guard is better than nothing while you wait for a dental appointment, but a custom-fitted guard from your dentist is far more effective.
- If the tooth was ground down during a dental procedure, do not pick at it or test it obsessively with your tongue. Let it settle, but track your symptoms carefully.
When to call the dentist today
You should book an appointment today (not next week) if you have any of the following: persistent or worsening pain after a dental procedure that involved grinding, spontaneous throbbing that wakes you up at night, pain that lingers more than 30 seconds after a temperature stimulus, visible cracking or chipping, swelling, or any sign of an abscess. If you just have mild sensitivity after minor tooth contouring with no pain on biting and no spontaneous aching, you can monitor for a week or two with the self-care steps above before scheduling a routine visit. When in doubt, call anyway. A quick phone triage with your dentist's office takes five minutes and can tell you whether to come in urgently or wait.
What a dentist can actually do to fix it
When you go in, your dentist will assess the depth of the damage through visual exam, x-rays, and sensitivity tests. What they recommend depends on how much tissue was removed and the current state of the pulp. Here is what the treatment ladder looks like:
- Fluoride varnish or remineralizing agents: for very early, superficial enamel erosion. Applied in office, they give the remineralization process a concentrated boost.
- Dental bonding: a tooth-colored resin is applied to rebuild minor chips or thinned surfaces. Not permanent, but it protects the exposed dentin and restores shape. Usually the first-line option for moderate grinding damage.
- Veneers: thin porcelain or composite shells bonded to the front of teeth. Good for multiple front teeth that have been worn down.
- Crowns: when grinding has removed significant tooth structure, a crown caps and protects what remains. This is often the right call after heavy wear or aggressive crown prep that has left dentin vulnerable.
- Direct pulp capping: if the pulp is minimally exposed during a procedure, the dentist places a biocompatible material (often mineral trioxide aggregate) directly over the exposure to encourage reparative dentin formation and preserve pulp vitality.
- Root canal: if the pulp is infected, dead, or too severely damaged to respond to capping, a root canal removes the pulp tissue, cleans the canal, and seals it. The tooth is then typically restored with a crown.
- Night guard (custom): if bruxism caused the damage, a lab-fabricated custom guard is the most important long-term preventive step. It will not regrow what was lost, but it prevents further loss.
Recovery timelines vary. Sensitivity after bonding or crown placement often settles within two to four weeks. Pulp capping outcomes are evaluated at follow-up appointments, sometimes over six to twelve months, because the pulp's response to reparative dentin formation takes time. If symptoms worsen instead of improving after any of these procedures, that is a signal to go back in.
Age matters: kids, teens, and the 'wait, did it grow back?' confusion
Children and baby teeth
Kids present a genuinely different situation. Baby (primary) teeth are placeholders, and permanent teeth are developing underneath them. If a child's tooth gets ground down from bruxism or a dental procedure, the primary tooth itself does not regenerate, but the permanent tooth beneath is still coming. This is different from whether dentin can grow back after it has been removed by grinding or other dental procedures dentin grow back. This can create a confusing appearance where it looks like the tooth 'grew back' after some time, when in reality the permanent tooth simply erupted on its natural schedule. If you are a parent watching this happen, it is reassuring but not magical: it is just normal eruption. What matters is whether the ground-down baby tooth caused problems (infection, alignment issues) before the permanent tooth arrived.
Teens and young adults
Teenagers still developing their permanent dentition have more at stake when enamel is lost. Their enamel is fully formed on erupted teeth but the teeth may still be in the process of fully maturing (posteruptive maturation), which means remineralization strategies are somewhat more effective in teens than in older adults. This does not mean lost enamel grows back, but it does mean fluoride and remineralizing toothpastes can have a more meaningful protective impact during this window. That means answers to “can enamel grow back” are generally no, but treatment can still help protect and restore the tooth lost enamel grows back. Bruxism in teens is also common and frequently goes untreated because it seems less serious, but the cumulative damage adds up quickly.
Adults and continued eruption confusion
Adults sometimes notice a tooth looks slightly longer or has shifted after grinding, and they wonder if the tooth somehow grew. What is more likely happening is that the opposing tooth (or surrounding teeth) have drifted or erupted slightly in response to changes in bite pressure, a well-documented phenomenon called super-eruption or passive eruption. The tooth did not regrow; the bite dynamics shifted. This is worth mentioning to your dentist because drift can create new problems, including further uneven wear.
A note on root and bone
Grinding effects are not always limited to what you can see. Severe chronic bruxism puts pressure on tooth roots and the surrounding bone. Small, localized damage to the root surface (cementum) can sometimes repair on its own within a few weeks if the stimulus is removed. If you are wondering whether tooth roots can grow back after grinding damage, the answer is usually no and depends on how much root and supporting tissue was affected. However, damage affecting more than about 20% of the root surface can cause extensive cell death and will not heal spontaneously. This is another reason stopping the grinding source and getting a proper evaluation matters beyond just the crown of the tooth. The question of whether bone and root structures can regenerate is its own complex topic, and the short answer for both is: only partially, only under specific conditions, and not in a way that substitutes for treatment. Bone and root regeneration after grinding is limited, so in most cases you cannot expect can bone grow back around teeth to replace lost tooth structure.
The bottom line on realistic expectations
Grinding removes tooth structure that your body cannot fully replace. The biological ceiling here is real and not something supplements, special toothpastes, or internet remedies will change. What you can do is stop further damage immediately, support whatever limited remineralization is possible at the surface level, manage sensitivity with evidence-backed products, and get a dentist's assessment so you know what you are actually dealing with. The good news is that modern dentistry has excellent tools for restoring function and appearance after grinding damage, from bonding and veneers to crowns and beyond. The teeth themselves will not regrow, but with the right treatment, you can get back to a tooth that looks, feels, and functions normally.
FAQ
If enamel cannot regrow, why do some people say their “worn teeth came back” after changing toothpaste or habits?
Most of what people notice is either reduced sensitivity as microscopic surface demineralization reverses, or a visible improvement from stain removal and smoothening after dental work. It can also be true that the opposite tooth shifted, making the worn tooth look more even, or that a child’s permanent tooth simply erupted later. True regrowth of physically ground enamel is not what is happening.
Can whitening or “enamel repair” products make ground-down teeth thicker again?
Whitening can lighten discoloration but does not rebuild missing enamel thickness. “Enamel repair” claims generally refer to remineralization of early surface damage, not replacing enamel that has been worn down by measurable grinding or tooth contouring. If you see a noticeable flat or thin spot, expect protection and restoration, not regrowth.
What’s the fastest way to stop grinding from getting worse while I wait to see the dentist?
Use a dental night guard if you have one, and avoid hard or sticky foods that increase bite stress (nuts, ice, chewy candy). Also track when sensitivity happens, morning versus night, because it helps your dentist judge whether the grinding is active and how aggressive the wear likely is.
Is mild sensitivity after grinding normal, and when should I treat it as a red flag?
Mild, short-lived sensitivity after minor contouring can settle within weeks, especially if bite pain is absent. Treat it as urgent if pain is spontaneous (not just triggered), worsening over days, if you feel sharp pain when biting, or if you develop swelling, bad taste, or night-throbbing pain.
If I ground my tooth with “no drilling” contouring or a kit at home, can the tooth heal by itself?
Home grinding or aggressive filing removes enamel and can also damage dentin, sometimes pushing the tooth toward exposed dentin or even pulp irritation. Unlike small reversible surface changes, these effects are usually not self-correcting. You should get an exam to check depth, cracks, and pulp status.
How do dentists decide between fluoride-only care versus bonding, crowns, or root-canal treatment?
They base it on wear depth, whether dentin is exposed, crack presence, and pulp health. Tests often include bite and percussion assessment, x-rays for hidden problems, and thermal or cold sensitivity tests. If symptoms suggest pulp involvement or a crack is progressing, you may need restoration or pulp therapy rather than just remineralization.
If dentin can sometimes form reactionary or reparative dentin, does that mean the tooth fully regains what was removed?
No. Dentin response can create a protective bridge and reduce progression, but it does not recreate the original enamel thickness or restore the lost shape. The result is often partial stabilization, which is why follow-up timing matters (sometimes months) and why the pulp may still fail if injury is too deep or treatment is delayed.
Can a tooth look longer after grinding and not be “regrowing”?
Yes. Changes in bite dynamics can cause neighboring teeth to drift or erupt slightly (super-eruption or passive eruption). That can make the worn tooth appear longer even though it did not grow. Tell your dentist so they can evaluate occlusion and prevent uneven wear from continuing.
Does grinding damage the root and bone, and what symptoms would suggest that?
It can in severe chronic bruxism, but you often will not feel it directly at first. Symptoms that raise concern include persistent or deep aching, mobility, pain on biting that feels different from simple sensitivity, and signs of infection. If grinding is severe, an x-ray review and bite assessment are important even if the surface looks only mildly worn.
If the pulp is close to the surface, how quickly should I seek care after a procedure that involved grinding?
If you have escalating pain, pain that wakes you up at night, pain that lasts unusually long after a cold or hot stimulus, or visible chipping or cracks, seek evaluation promptly rather than waiting. For minor contouring with only mild sensitivity that is steadily improving, a short observation period can be reasonable, but “worsening” should always shorten the timeline.
Realistic timelines for enamel repair: early remineralization days to months, no true regrowth in adults, plus next step
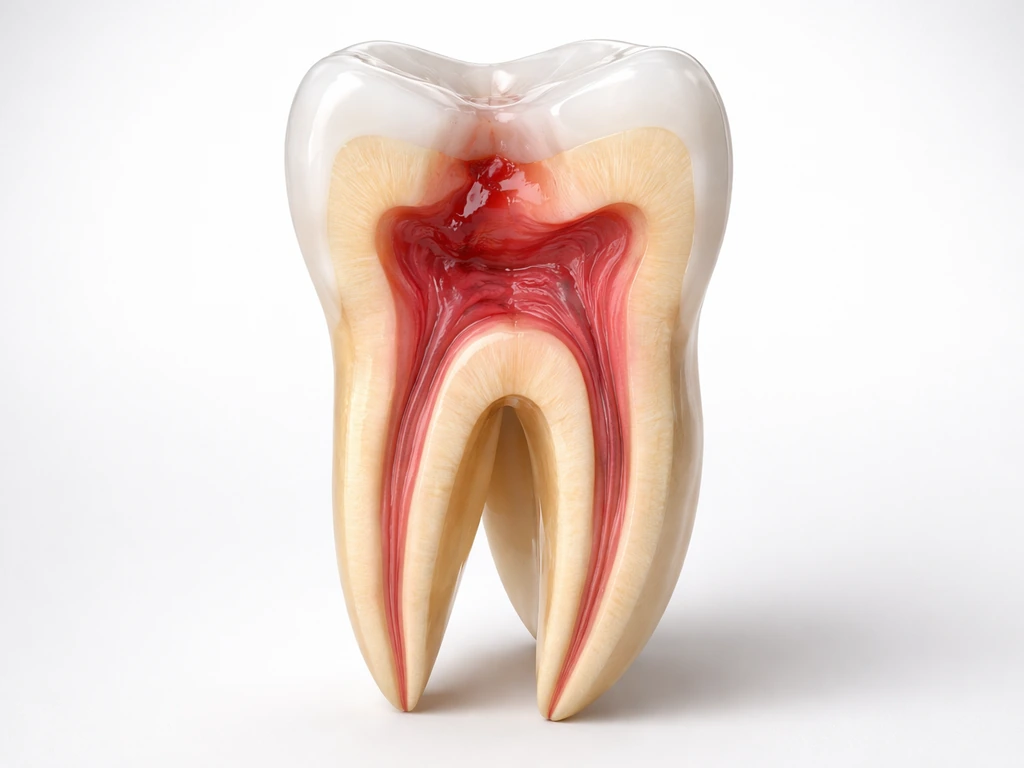
Can tooth nerves regrow? Learn if pulp can recover by age and damage stage, and what treatments you need.
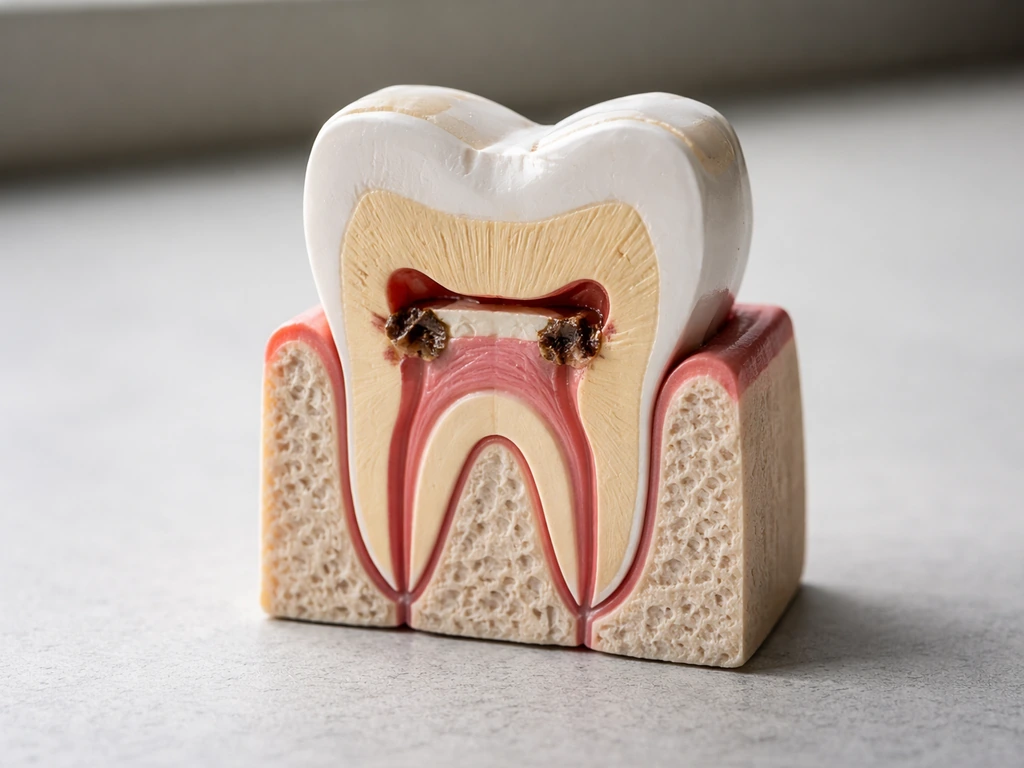
Yes or no on dentin regrowth, realistic timelines, and what to do for exposed dentin, cavities, trauma, and repair optio

