Here's the direct answer: adults cannot naturally grow a brand-new tooth. Once your permanent teeth are in, your body has no built-in program to manufacture a replacement tooth from scratch. That's not pessimism, that's just how human dental biology works. But the question "how to grow new teeth" actually covers a few very different situations, and depending on your age and what's going on in your mouth, the answer gets more nuanced. In contrast, what helps teeth grow in children depends on normal development and good oral health habits rather than regrowing a missing adult tooth. Some things can regenerate to a degree. Some things never will. And for the rest, there are real clinical options that can restore function and appearance even when biology won't cooperate.
How to Grow New Teeth: What’s Possible and Next Steps
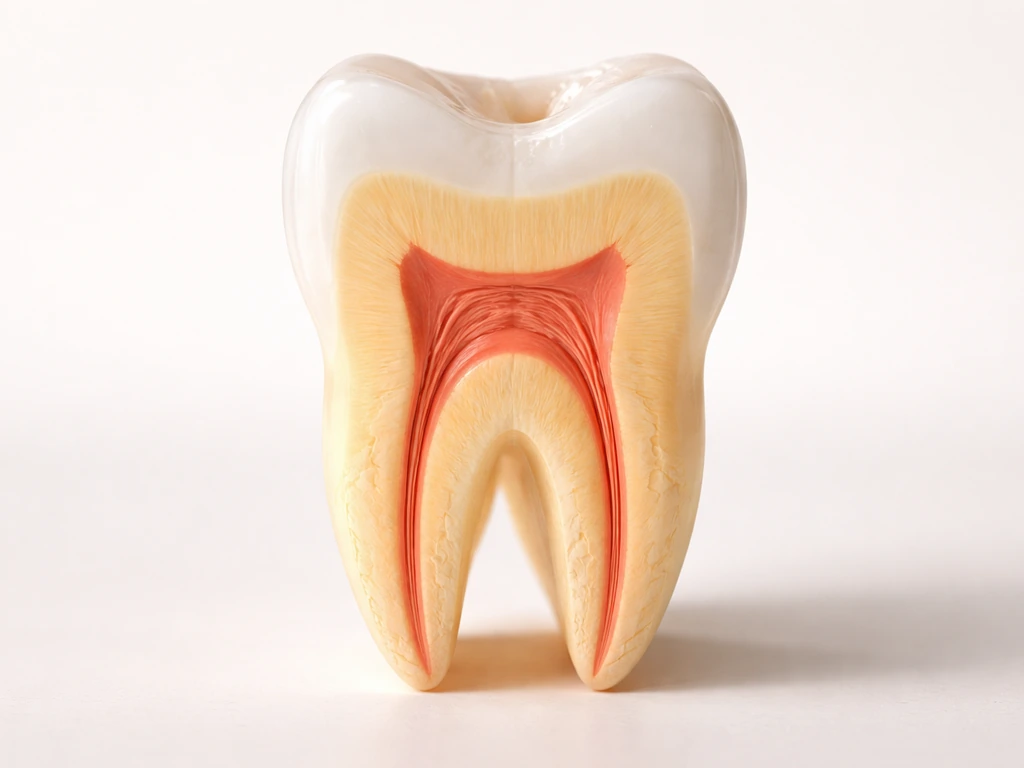
What people mean when they say "grow new teeth"
The phrase covers at least three completely different things, and it's worth sorting them out before going any further, because the answers are totally different for each.
- True tooth regeneration: the idea that a lost or extracted adult tooth could regrow biologically, complete with enamel, dentin, pulp, and a root attached to the jaw via a periodontal ligament. This is what most people searching the phrase are hoping for.
- Eruption of a developing tooth: a tooth germ that already exists in the jaw but hasn't come through the gum yet. Wisdom teeth are the most common example. If you're asking because a new tooth seems to be appearing in the back of your mouth, this is probably what's happening.
- Dental restoration or replacement: using implants, bridges, or dentures to replace a missing tooth. This isn't biological regrowth, but it does restore the function and look of a natural tooth, and it's what dentists actually recommend when a tooth is gone.
A lot of the confusion online comes from mixing these three up. Someone sees a headline about stem cell research and assumes a pill to grow a new tooth is around the corner. Someone else notices pressure in their lower jaw and wonders if a tooth is "growing." These are fundamentally different situations requiring different conversations.
What science actually says about regrowing teeth
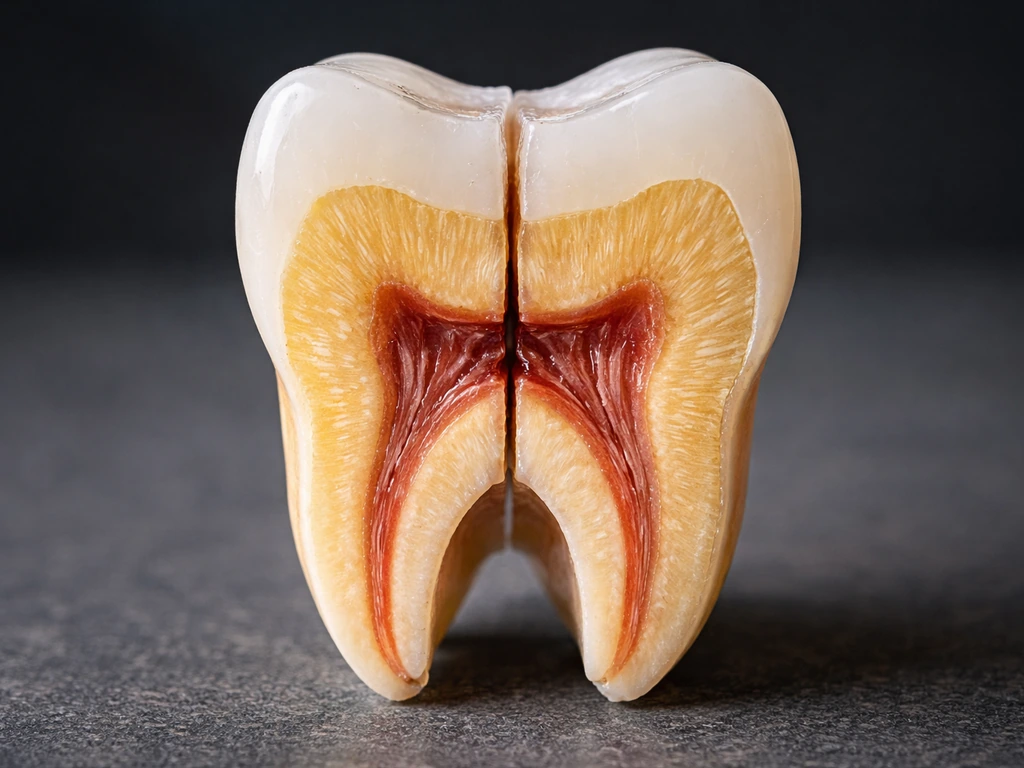
Let's go structure by structure, because each one behaves differently when it comes to regeneration.
Enamel
Enamel is the hardest tissue in the human body, and once it's gone, it's gone. The cells that form enamel (ameloblasts) are lost after a tooth erupts, so there's no cellular machinery left to rebuild it. You can remineralize very early enamel surface damage with fluoride and good saliva conditions, but that's reinforcing and hardening existing enamel crystals, not growing new enamel. A cavity that has breached enamel won't fill itself back in. This topic connects closely to questions about enamel regrowth specifically, which is a subject with its own nuances worth digging into.
Dentin
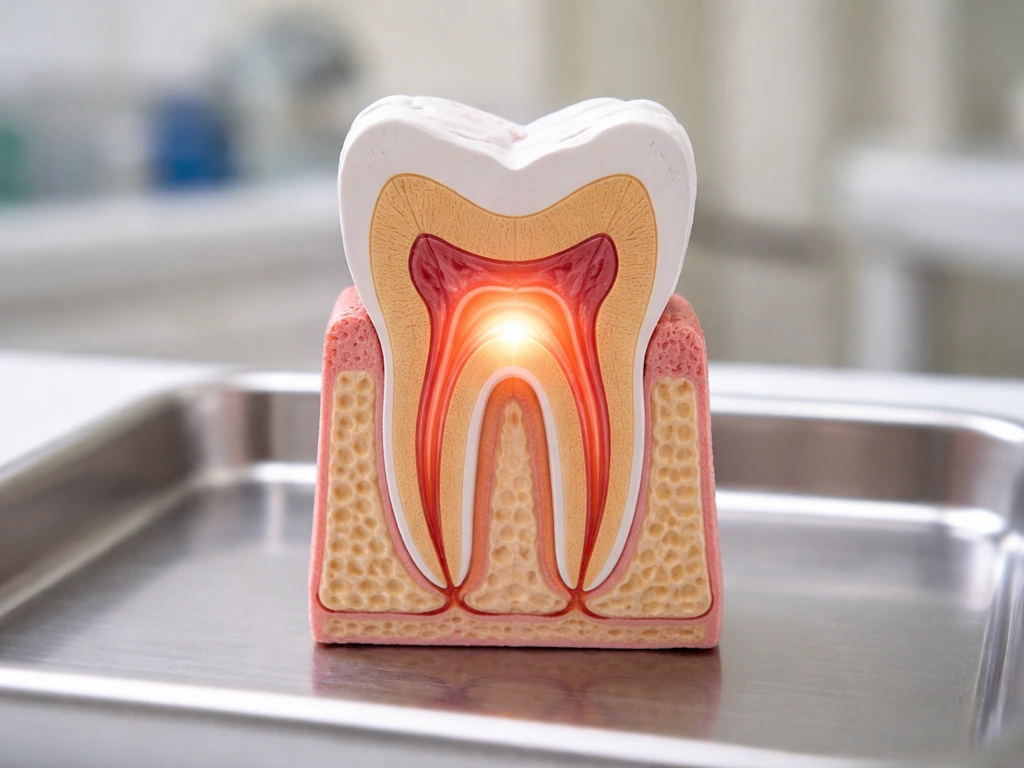
Dentin has a little more flexibility. Odontoblasts (the cells that lay down dentin) can produce what's called tertiary or reparative dentin in response to mild irritation or decay. Your tooth is essentially trying to wall off a threat. But this is a defensive response, not meaningful regeneration. It doesn't restore the original tooth structure and doesn't happen when a tooth is already lost.
Pulp
There's genuine research interest in pulp regeneration, particularly for younger patients whose tooth roots haven't finished forming. Regenerative endodontic procedures can, in specific cases with immature teeth, encourage continued root development. For adults with mature roots, though, the evidence is limited, and conventional root canal treatment remains the standard approach. The clinical takeaway: pulp regeneration in adult permanent teeth is not a widely available or proven clinical option today.
Roots and periodontal attachment
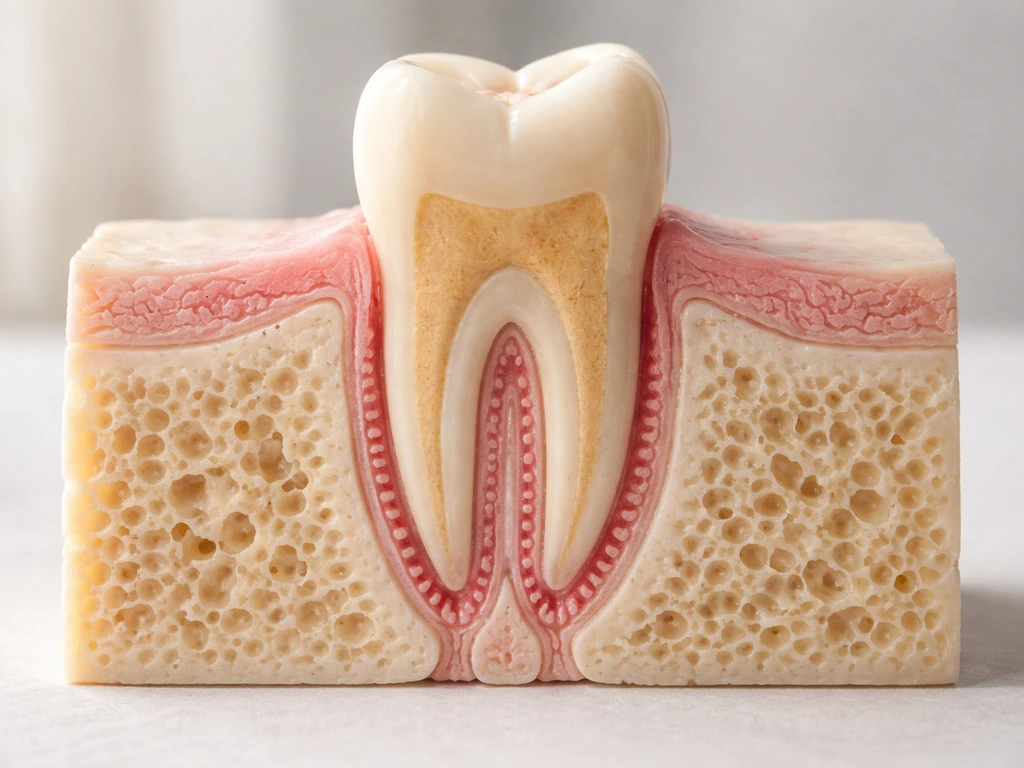
Root formation during development involves a structure called Hertwig's Epithelial Root Sheath, which coordinates the complex signaling needed to build a root and its attachment apparatus. Once that developmental window has closed in adulthood, that process cannot simply be restarted. Guided Tissue Regeneration (GTR) and bone grafting can repair and partially restore periodontal defects so that an existing tooth has better support, but these procedures are rebuilding around a tooth that's already there, not generating a new root where there isn't one.
What about stem cells?
Yes, research into dental stem cells and tissue engineering is genuinely exciting. Studies have demonstrated that dental mesenchymal stem cells can form some dental-like tissue in experimental settings. But recreating the full developmental program needed to produce a whole organized tooth, with correct enamel, dentin, pulp, root, and a functioning periodontal ligament, is not something any clinic anywhere can currently do in a human patient. Clinical trials are exploring cell-based approaches, but "currently in research" and "available to you today" are very different things. Don't let a wellness website convince you otherwise.
Your age and situation change everything
The first practical step is figuring out which category you're actually in, because the path forward is completely different depending on your situation.
| Situation | What's probably happening | What's actually possible |
|---|---|---|
| Child under 12 with a loose or missing tooth | Baby tooth falling out; permanent tooth developing underneath | Permanent tooth will erupt naturally; support with good nutrition and oral hygiene |
| Teen or young adult (17–25) with pressure or swelling in the back of the mouth | Wisdom teeth (third molars) erupting or becoming impacted | Tooth may erupt on its own; X-ray needed to check positioning and space |
| Adult with a damaged (cracked, decayed) tooth still in the socket | Existing tooth needs repair; some supporting tissue may be regenerable | Repair via filling, crown, or root canal; GTR or bone graft if periodontal involvement |
| Adult with a fully extracted or knocked-out tooth | Tooth germ is gone; no biological regrowth possible | Implant, bridge, or denture are the replacement options |
| Adult noticing gum recession or loose teeth | Periodontal disease affecting bone and attachment | Professional periodontal treatment; GTR in selected defects; cannot reverse all bone loss naturally |
A note on wisdom teeth specifically

Third molars typically erupt between ages 17 and 25, though timing varies widely. If you're in that age range and a tooth seems to be coming in at the very back of your mouth, it might genuinely be a new tooth arriving, just one that was always there developing in the jaw. The catch is that wisdom teeth are often impacted, meaning there isn't enough space for them to erupt fully or correctly. A dental X-ray is the only reliable way to know whether a wisdom tooth is positioned well enough to come through or needs evaluation for removal.
What you can actually do naturally to help
Here's where I want to be honest about what "natural" support can and cannot do. No supplement, oil pull, herbal rinse, or dietary protocol will regenerate a lost tooth. Full stop. But the condition of your gums, jaw bone, and surrounding tissue absolutely affects whether existing teeth stay healthy, whether restorative procedures succeed, and whether any regenerative clinical work holds up over time. So this matters, just not in the magical way some websites imply.
What genuinely helps
- Control inflammation: brushing twice a day and flossing reduces gingival inflammation, which is the foundation of periodontal health. Chlorhexidine mouthrinse has solid evidence for reducing gingivitis as an adjunct, though it's not a long-term daily substitute for mechanical cleaning.
- Quit smoking: tobacco use is one of the strongest predictors of periodontal disease progression, tooth loss, and poor healing after dental procedures. Stopping smoking meaningfully improves how your gums and bone respond to treatment.
- Support bone and gum nutrition: adequate calcium, vitamin D, and vitamin C all support the tissues that hold teeth in place. These aren't magic nutrients, but deficiencies genuinely impair healing.
- Stay on top of professional cleanings: biofilm and calculus below the gumline cannot be removed at home. Regular cleanings prevent the chronic infection that destroys bone.
- Manage systemic conditions: diabetes and immune conditions directly affect periodontal healing. Working with your GP on blood sugar control, for example, has a real measurable impact on gum disease outcomes.
What won't help (and what to avoid)

- Supplements or products marketed as "tooth regrowth" formulas: there is no clinical evidence any over-the-counter product can regrow a missing tooth.
- Delaying treatment: waiting to see if a lost or severely damaged tooth fixes itself only allows bone loss to progress, which reduces your options later.
- Aggressive at-home abrasives: whitening products and abrasive toothpastes won't help and can damage existing enamel further.
- Ignoring pain or pressure: especially in the wisdom tooth area, untreated impaction can damage neighboring teeth and cause infection.
When you need professional help (and what that looks like)
If a tooth is missing or severely compromised, a conversation with a dentist is not optional, it's the starting point for every real path forward. Here's what that process typically involves.
- Clinical exam: the dentist checks what teeth are present, their condition, the health of surrounding gum and bone, and whether there's any sign of active infection or disease.
- Imaging (X-rays or CBCT): a periapical X-ray or cone beam CT scan shows the bone level around teeth, whether any unerupted teeth exist in the jaw, and the quality of the bone available for implant placement.
- Periodontal assessment: if gum disease is involved, a periodontist evaluates pocket depths, bone loss patterns, and whether GTR or bone grafting could help stabilize or improve supporting structures.
- Restorative planning: for a missing tooth, the options typically come down to a dental implant (titanium post placed in the jaw, with a crown on top), a fixed bridge (using adjacent teeth as anchors), or a partial or full denture. Each has different requirements, costs, timelines, and tradeoffs.
- Regenerative endodontic evaluation: if you have a damaged but not yet lost tooth, especially a younger patient with an immature root, an endodontist can assess whether regenerative endodontic treatment is appropriate.
The earlier you see a professional after a tooth is lost or damaged, the more options you have. Bone begins to resorb within weeks of tooth loss, and the window for certain implant approaches narrows as bone volume decreases. This is not meant to scare you, just to be clear that time genuinely affects your choices.
Your practical next steps, right now
Based on everything above, here's how to move forward depending on where you are today.
If you're a parent of a child with a missing or slow-to-arrive tooth
For kids under 12, patience is usually appropriate as permanent teeth develop on their own schedule. If a baby tooth was lost early due to decay or trauma, ask the dentist about a space maintainer to prevent neighboring teeth from drifting and crowding out the incoming permanent tooth.
If you're 17–25 and feel something happening in the back of your mouth
Book a dental appointment and ask for an X-ray of your third molars. You need to know whether they're positioned to erupt cleanly, partially impacted, or fully impacted. Do not ignore persistent pain, swelling, or difficulty opening your mouth in that area.
If you're an adult with a tooth that's damaged but still in your mouth
Get it evaluated as soon as possible. A tooth that can be saved is almost always worth saving. Ask the dentist directly: "Can this tooth be restored, and for how long?" and "Is there any periodontal involvement that needs treatment first?" If the tooth is borderline, a second opinion from an endodontist or periodontist is reasonable.
If you're an adult with a tooth that's already gone
Ask your dentist: "Do I have enough bone for an implant, and if not, is a bone graft feasible?" and "What are the long-term tradeoffs between an implant, a bridge, and a partial denture for my specific situation?" These are the right questions because the answers depend heavily on your bone volume, the location of the missing tooth, adjacent tooth health, and your budget.
Red flags that should prompt an urgent appointment
- Swelling in the jaw or face, especially with fever: this can indicate a spreading dental infection and is a same-day or emergency situation.
- A tooth that was knocked out within the last hour: a knocked-out permanent tooth may be reimplantable if you act within about 30 to 60 minutes. Keep it moist (in milk or between your cheek and gum) and get to a dentist immediately.
- Sudden loosening of multiple teeth: this can indicate aggressive periodontal disease or a systemic issue and needs prompt evaluation.
- Persistent numbness or pain along the jaw after a tooth extraction: this warrants follow-up to rule out nerve involvement or dry socket.
Realistic expectations to carry with you
It helps to be honest with yourself going into this. If you're an adult who lost a tooth, no current natural method will grow it back. You might also be wondering whether milk helps your teeth grow, but tooth growth and repair depend more on your dental biology and habits than on any single food does milk help your teeth grow. In practical terms, that means figuring out what enamel damage you have and focusing on prevention and remineralization rather than true regrowth grow back enamel. What you can do is protect the teeth you have, support the bone and gum tissue around them, and work with a dental professional to replace what's missing in a way that looks, feels, and functions well. If you are worried that your teeth are small, a dentist can also help you understand whether normal growth or orthodontic treatment is needed my teeth are small will they grow. The science of dental regeneration is genuinely advancing, including work on enamel remineralization, periodontal tissue repair, and stem cell-based approaches, but none of that changes what's available to you in a clinic today. The most useful thing you can do right now is get an accurate picture of your specific situation from a professional, because the right plan is completely personal to your anatomy, your history, and your goals.
FAQ
If I’m missing a tooth, are there any vitamins or supplements that can actually regrow it?
No. For adults, no supplement can trigger true regrowth of a missing tooth. The practical role of nutrition is supporting gum and bone health for the success of restorations like implants or grafting, so focus on addressing deficiencies if you have them (with a clinician), rather than expecting regrowth.
How can I tell whether what I feel is a new tooth erupting versus pain from something else?
Eruption-related changes are usually slow and localized, while tooth pain with swelling, fever, or worsening bite pain often points to infection or impaction issues. An X-ray is the quickest way to distinguish “something is coming in” from “there’s a problem around an existing tooth or trapped tooth,” especially for wisdom teeth.
Can enamel “grow back” if my cavity is small?
If the damage is very early and confined to surface enamel, fluoride and saliva support can reverse mineral loss and strengthen the surface. But once a cavity has formed through enamel, it will not refill itself, and you generally need a filling or other restorative approach to stop progression.
Does dental stem cell treatment mean I can get a full new tooth soon?
Not in routine clinical care today. Research shows cells can sometimes create dental-like tissue in controlled studies, but rebuilding the complete system (enamel, dentin, pulp, roots, and periodontal ligament) with predictable function is not yet a standard, widely available option for patients.
Is a tooth “saved” more often if I see a dentist quickly after damage or loss?
Yes. For tooth loss, bone resorption can start within weeks, which can narrow implant options later. For damaged teeth, early evaluation can sometimes preserve structure or slow deterioration before the tooth becomes non-restorable, so prompt care expands choices.
If I lost a tooth, how do I decide between an implant, bridge, or partial denture?
The decision mainly depends on bone volume and adjacent tooth condition. Implants may require enough bone or grafting, bridges rely on preparing neighboring teeth, and partials are removable and can be useful when bone restoration is not feasible. Your dentist should compare longevity, maintenance, comfort, and cost for your specific area (front versus back) and bite mechanics.
What should I ask about bone grafting if I want an implant?
Ask whether you need a graft to increase width, height, or both, how the graft affects the timeline to implant placement, and what the success rates look like in your case. Also ask what happens if the graft does not integrate as planned, so you understand backup options.
If I had root canal treatment, can regeneration happen afterward?
Regeneration is not the default outcome of root canal therapy in adults. What clinicians can do is remove infected tissue, disinfect the system, and then monitor healing. If a tooth has immature roots (more common in children), regenerative endodontics may be considered in selected cases, but this is different from adult mature-root teeth.
Could “space maintainers” help prevent adult tooth issues after early baby tooth loss?
They can. If a baby tooth is lost early, neighboring teeth may drift and reduce space, increasing the odds of crowding when permanent teeth erupt. A space maintainer can help preserve the eruption path, and the dentist or orthodontist can tell you whether it’s needed based on your child’s situation.
Are home remedies like oil pulling or herbal rinses useful if I’m trying to regrow teeth?
They cannot regrow a lost tooth. Some practices may modestly support oral comfort or hygiene, but they should not replace evidence-based prevention, professional care, and treatment. If you have pain, swelling, or a suspect cavity, home remedies should be considered supportive only, not a substitute for diagnosis and treatment.
Learn what enamel can’t regrow, how to reverse early loss with fluoride and diet, and when dentist repair is needed.
Learn what can regrow after tooth loss, what cannot, and next steps to rebuild gum and support bone safely.
Learn what works to strengthen enamel and partially remineralize it, plus what can’t regrow and a daily routine.

