Teeth don't actually "grow" through your gums the way a plant pushes through soil. What's really happening is that the tooth is already fully (or mostly) formed beneath your gums, inside the jawbone, and it's migrating upward through the tissue until the crown pokes into your mouth. That distinction matters, especially if you're wondering whether a tooth can somehow regrow after it's been lost or damaged. The short answer: no, it can't. But let's walk through exactly what does happen, what's normal at every age, and what to do if something seems off.
How Do Teeth Grow Through Gums: Eruption Timeline
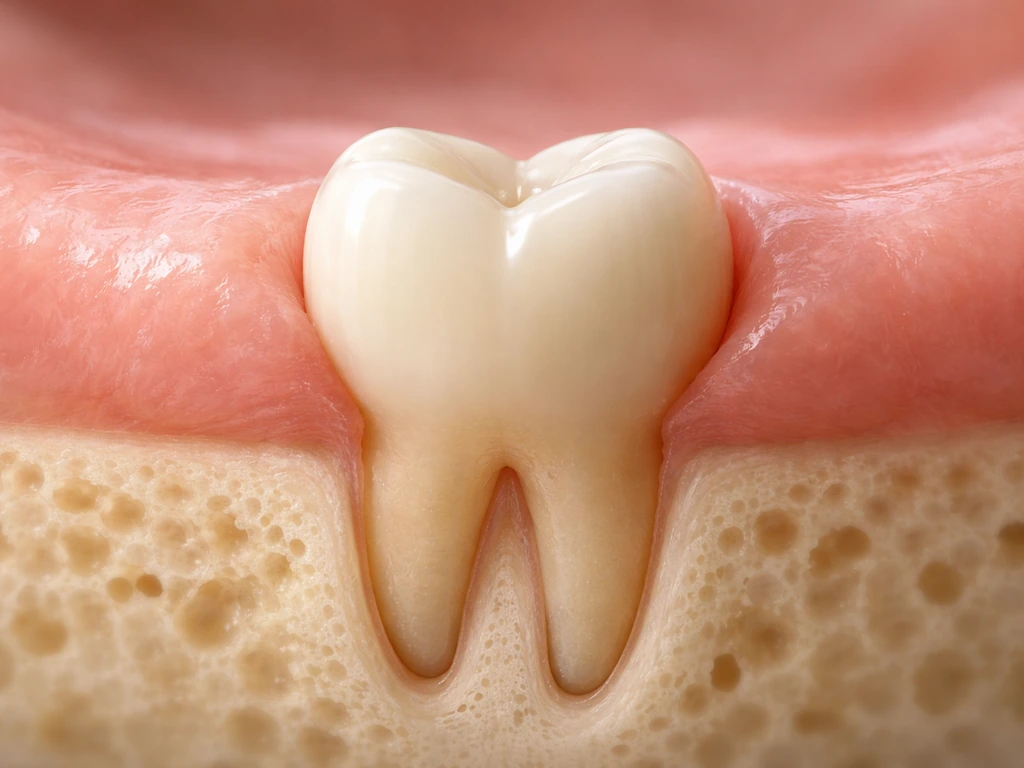
What "growing through the gums" actually means
The term "eruption" is what dentists use, and it's more accurate than "growing." Tooth eruption is the process by which an already-formed tooth moves through the jawbone and gum tissue into the oral cavity. By the time you see any hint of a tooth at the gumline, that crown has been quietly developing for months or even years. The tooth doesn't form at the surface and push down; it forms deep in the jaw and travels up.
As the tooth makes its upward journey, the surrounding structures adapt. The periodontal ligament, cementum, and alveolar bone all form and organize around the developing root, anchoring the tooth in place once it arrives in the mouth. So eruption isn't just a tooth popping through a hole; it's a coordinated biological event involving the tooth, the bone around it, and the soft tissue above it. If you've ever been curious about where teeth actually originate inside the jaw before they ever appear, the answer involves specialized cells and structures laid down before birth.
Tooth development from the very beginning
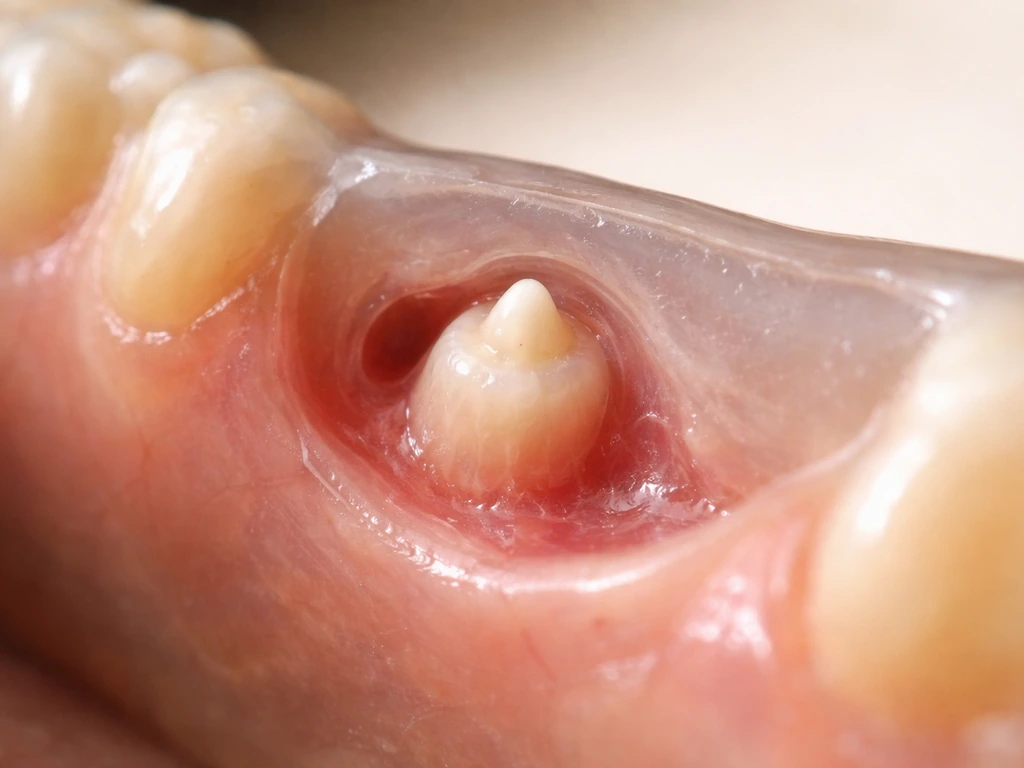
Tooth development starts surprisingly early. Tooth buds begin forming at around 6 weeks in utero, which means your teeth were technically in progress before you were even born. Dentin is produced by cells called odontoblasts, and enamel is laid down by ameloblasts. These two cell types are doing completely different jobs, forming distinct layers of the same tooth. Primary (baby) teeth typically start erupting around 6 months after birth, with the full set of 20 baby teeth usually in place by age 3.
Permanent teeth follow a much longer timeline. If you want a full picture of how teeth grow from bud to eruption, the biology is genuinely fascinating: the same basic sequence repeats for every tooth, just offset in time. Root development, worth noting, continues after a tooth has already emerged into the mouth. The root isn't finished when the crown appears; the tip of the root (the apical foramen) keeps narrowing for months or years after eruption. That's especially relevant for wisdom teeth, where root completion timelines are highly variable.
Eruption timelines by tooth type
| Tooth Type | Primary (Baby) Eruption Age | Permanent Eruption Age |
|---|---|---|
| Central incisors | 6–12 months | 6–8 years |
| Lateral incisors | 9–13 months | 7–9 years |
| Canines (cuspids) | 16–22 months | 9–12 years |
| First molars | 13–19 months | 6–7 years |
| Second molars | 25–33 months | 11–13 years |
| Third molars (wisdom teeth) | N/A | 17–25 years (highly variable) |
Wisdom teeth deserve special mention because they have the widest range of any tooth. The commonly cited window is 17 to 25 years, but panoramic X-ray studies show that gingival emergence can span from the late teens well into the early 20s, with some differences between males and females. Some people's wisdom teeth never erupt at all, either because there isn't enough room or because the teeth are angled in a way that blocks their path completely.
What actually controls eruption: roots, bone, and gum changes
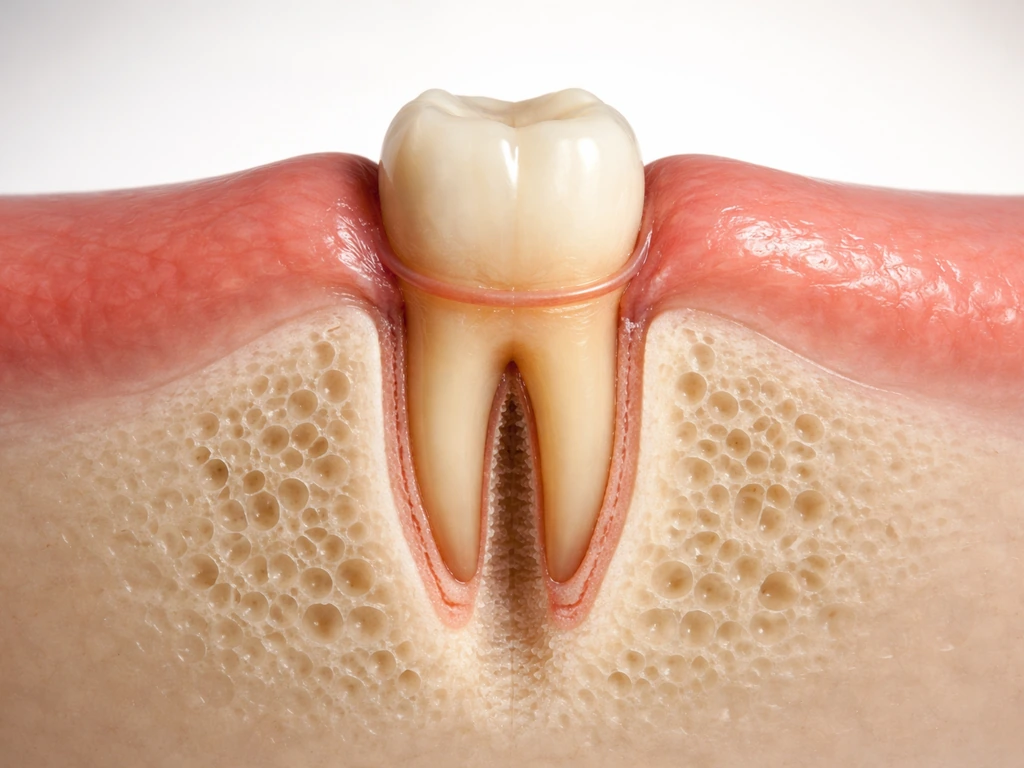
Eruption isn't random. The dental follicle, a sac of tissue surrounding the developing tooth, plays a key coordinating role. It sends signals that trigger bone resorption in front of the erupting tooth and bone deposition behind it, effectively creating a pathway through the jaw. Osteoclasts (the cells that break down bone) are activated in the bone above the tooth, while new bone forms below. This continuous remodeling is what allows the tooth to travel upward without the jaw falling apart.
The periodontal ligament also contributes to the mechanics of eruption. As the root develops and the ligament fibers organize, they help guide and anchor the tooth during its final positioning. The gum tissue directly above an erupting tooth thins and eventually splits, which is why you sometimes see a slightly bluish, fluid-filled bump (called an eruption cyst) right before a tooth breaks through. That bump usually resolves on its own without treatment.
The regrowth myth: what teeth actually can and cannot do
This is where a lot of internet misinformation lives, so let's be direct. Eruption is not regrowth. A tooth moving through your gums was already there, already formed, just waiting to emerge. It is not a new tooth being created. Once a permanent tooth is lost, there is no third set waiting in the wings. Humans are diphyodont, meaning we get exactly two sets of teeth, and that's it biologically.
Beyond tooth loss, the individual structures of a tooth also cannot regenerate once they're damaged or destroyed. Enamel is the hardest substance in the human body, but once it's gone, it's gone. Ameloblasts, the cells that built your enamel, are no longer present after a tooth erupts. There's no mechanism to rebuild enamel naturally, which is exactly why cavities can't simply "heal" the way a skin cut does. The same is true for dentin and cementum: these mineralized tissues do not self-regrow in any meaningful way after loss or damage. The pulp (the soft inner tissue) has some limited capacity for repair under very specific conditions, but we're talking about minor reactionary dentin formation, not anything close to regenerating an entire tooth. If you've seen claims online about oil pulling or supplements regrowing enamel, those claims have no biological basis.
This is also true of the tooth's supporting structures. After a tooth is lost, the periodontal ligament, the cementum, and the surrounding alveolar bone all begin to break down and resorb. That entire complex anchorage system disappears with the tooth, which is part of why replacing a lost tooth (especially with an implant) needs to happen sooner rather than later. There's a practical reason your dentist keeps bringing up bone loss.
When eruption goes wrong: signs that something's off
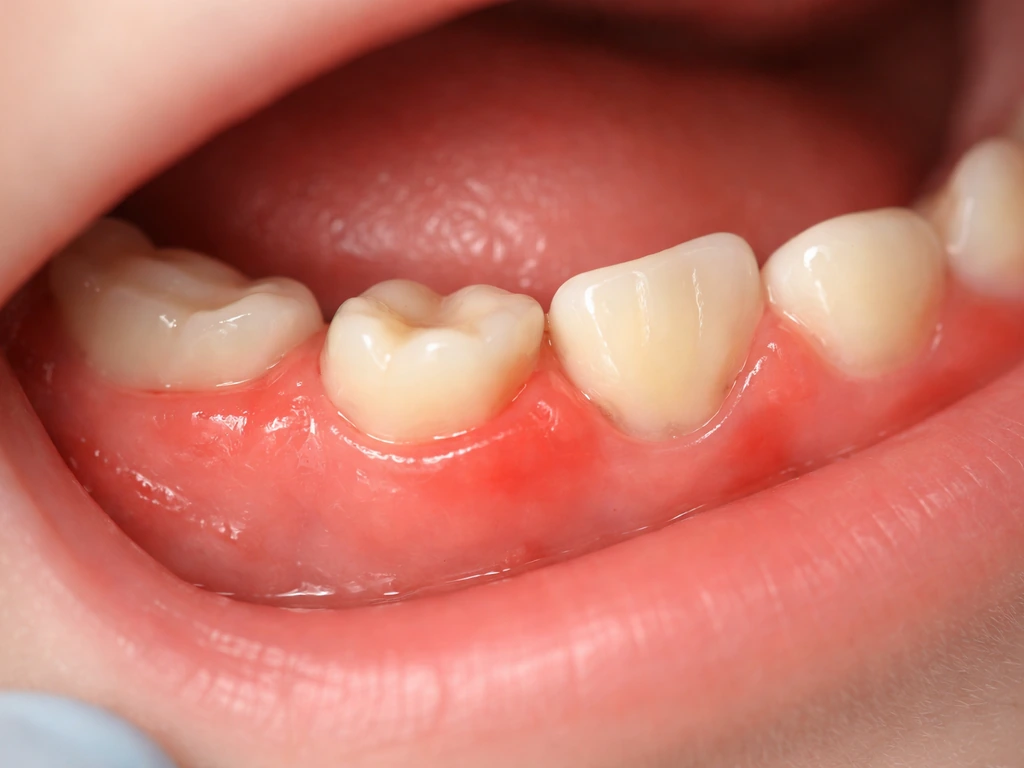
Most eruption is uncomfortable but normal. Some redness and swelling at the gumline, mild fussiness in infants, and general soreness are par for the course. But there are situations where eruption is genuinely abnormal and worth evaluating. Knowing the difference can save you a lot of unnecessary worry, or help you catch a real problem early.
One common scenario parents notice is when a permanent tooth appears to be coming in behind a baby tooth that hasn't fallen out yet. This is sometimes called "shark teeth" and while it looks alarming, it's often manageable. That said, understanding why teeth sometimes grow behind other teeth involves both eruption timing and root resorption of the baby tooth, and a dentist can tell you quickly whether the baby tooth needs to come out or whether waiting is fine.
Eruption problems can also stem from physical obstacles in the jaw: supernumerary (extra) teeth, cysts, or odontomas can block a tooth's path entirely. Ankylosis, where a tooth fuses to the surrounding bone, can cause a tooth to appear stuck or sunken relative to neighboring teeth as the jaw grows around it. These conditions are typically identified through X-rays, which is why routine dental imaging in children matters even when everything looks normal from the outside.
For wisdom teeth specifically, impaction is extremely common. An impacted wisdom tooth is one that simply cannot break through the gum, whether because it's angled sideways, blocked by the second molar, or there just isn't enough room in the jaw. Symptoms can include pain or tenderness at the back of the mouth, swelling around the jaw, and difficulty opening the mouth fully. These symptoms are worth taking seriously and getting evaluated promptly.
Red flags that need a dentist soon
- Persistent pain at the back of the jaw, especially if swelling is involved
- A tooth that appears to be coming in severely tilted or sideways
- A permanent tooth that hasn't appeared by the expected age (delayed eruption)
- A tooth that seems to be sinking below the level of neighboring teeth over time (possible ankylosis)
- Visible extra or duplicate teeth in the same area
- Repeated infections or gum swelling around a partially erupted wisdom tooth
- A child's permanent tooth erupting while the baby tooth is still firmly in place after several months
It's also worth keeping in mind that some eruption delays are completely normal variation, while others signal something worth investigating. If you've been wondering why your teeth haven't come in yet, the answer depends heavily on which teeth, your age, and what (if anything) is blocking them. That's a question worth bringing to a dentist with a current set of X-rays.
Managing eruption discomfort at home

For infants and toddlers going through primary tooth eruption, the discomfort is real but manageable. Gently rubbing the gum where the tooth is erupting for about 2 minutes at a time can help relieve pressure and soothe irritated tissue. A clean finger or a cool (not frozen) teething ring works well. If a child is very uncomfortable or fussy, age-appropriate doses of acetaminophen or ibuprofen are the recommended options, following dosing guidelines for the child's weight and age.
One thing to be clear about: do not use benzocaine-based teething gels or oral numbing products on children under 2 years old. The FDA has issued strong warnings about these products due to a risk of a serious and potentially fatal blood disorder called methemoglobinemia. Even in older children, the benefit is minimal and the risk is real. Stick to the rubbing and appropriate pain medicine approach instead.
For adults dealing with wisdom tooth eruption discomfort, warm saltwater rinses (about half a teaspoon of salt in 8 ounces of warm water) can reduce inflammation around a partially erupted tooth. Over-the-counter ibuprofen or acetaminophen can manage pain in the short term. Keeping the area clean is important because food easily traps around partially erupted third molars, raising infection risk. But home care is a bridge, not a solution, if there's an underlying impaction or infection.
For context on why some teeth end up emerging at awkward angles or positions in the first place, it helps to understand why teeth sometimes grow in crooked, since crowding and jaw size are often at the root of both misalignment and impaction problems.
When to book a dental appointment (and what to expect)
The American Academy of Pediatric Dentistry recommends that a child's first dental exam happen at the time of the first tooth eruption, and no later than 12 months of age. This isn't just about checking for cavities; it's about establishing a baseline for eruption monitoring. Catching delays, crowding, or obstacles early gives a dentist (or orthodontist) far more options than waiting until problems become obvious to the naked eye.
For adults concerned about wisdom teeth, an evaluation typically involves a clinical exam and a panoramic X-ray, which shows all four wisdom teeth, their angles, their root development, and how much room exists for eruption. This imaging is what separates "probably fine, let's monitor" from "this needs to come out."
Professional options when eruption is stuck or problematic
When a tooth isn't erupting on schedule or is causing problems, there are several pathways a professional might recommend, depending on the cause and the tooth involved.
For children with delayed eruption caused by a physical obstacle like a supernumerary tooth or odontoma, removing the obstacle is often enough to allow the delayed tooth to erupt on its own. Supernumerary teeth are more common than most people realize, and understanding why extra teeth develop in the first place is a question that involves genetics and developmental anomalies rather than anything a patient did wrong.
When an impacted tooth (most commonly a canine or wisdom tooth) is worth saving or moving into alignment, an oral surgeon can expose the tooth surgically by removing gum tissue and sometimes a small amount of bone over the crown. An orthodontic bracket is then bonded to the exposed tooth, and a chain or wire is used to gradually pull it into its correct position over months. This is called surgical exposure and orthodontic traction, and it works well for canines especially.
For wisdom teeth, the calculus is different. NICE guidance and AAOMS recommendations both center on whether pathology is present or developing. Removing impacted wisdom teeth is generally indicated when there's evidence of infection, cysts, damage to adjacent teeth, cavities that can't be restored, or resorption. Simply being impacted, without complications, may not require immediate extraction depending on the clinical picture. Your oral surgeon will assess the specific anatomy and risk factors. Given that some people develop discoloration issues with newly erupted teeth as well, it's worth knowing that why teeth sometimes come in yellow is a separate question related to enamel formation, not eruption timing.
Monitoring is also a legitimate option. Not every delayed or slow-erupting tooth needs intervention right away. A dentist may recommend taking a new X-ray in 6 to 12 months to see whether the situation has changed before deciding on a treatment path. The key is not ignoring it; leaving an impacted tooth unmonitored for years can allow problems to develop silently.
The bottom line is this: teeth "growing through gums" is really a carefully orchestrated migration that the body has been planning since before you were born. Eruption follows a biological script, it has real timelines, and it can run into real obstacles. What it is not is regrowth. If you lose a tooth or damage your enamel, that structure is gone and needs clinical management, not waiting for nature to fix it. When in doubt about whether what you're seeing is normal eruption or something that needs attention, a current set of X-rays and a dentist's eyes are the fastest way to get a real answer.
FAQ
If I lost a tooth, can a new one grow through the gum later?
No. Eruption is the tooth already formed in the jaw moving upward, so a tooth cannot “grow” back into existence after it’s been lost. If you notice a new bump at the gumline, it’s usually the crown emerging, not replacement tissue for a missing tooth.
Why can a permanent tooth appear behind a baby tooth that hasn’t fallen out yet?
Often, yes. When a permanent tooth is erupting behind a retained baby tooth, the permanent root is pushing forward while the baby tooth root resorbs over time. Dentists decide whether to remove the baby tooth or monitor based on X-rays of the baby tooth roots and the permanent tooth position.
How can I tell if delayed eruption is normal or if it’s truly stuck?
A tooth can look like it’s “under” the gum but still be erupting normally if only a small portion of the crown is visible and there’s no escalating pain, swelling, or fever. The deciding factor is whether symptoms are worsening or there are signs of infection, cyst-related swelling, or impaction on imaging.
What can I safely do at home for eruption pain, and when should I stop waiting?
It depends on the cause. For teething discomfort, gentle gum massage and a teething ring are reasonable. For adult or older-child pain from a partially erupted tooth, warm saltwater rinses and over-the-counter pain relief can help, but persistent pain, bad taste, or swelling usually means the area needs an in-person evaluation.
What eruption-related symptoms mean I should seek urgent dental care?
You should be more concerned if there is pus, fever, rapidly spreading swelling, trouble swallowing, or difficulty opening the mouth. Those can be signs of infection around a partially erupted tooth and should be assessed urgently rather than managed only with rinses.
Is an eruption cyst (blue bump) dangerous or just part of normal eruption?
Yes. Some people get an eruption cyst, a bluish or translucent bump that can look dramatic but often resolves on its own as the tooth breaks through. If the swelling grows, becomes very tender, or is associated with infection symptoms, it needs evaluation.
Can I safely help a stuck erupting tooth by brushing harder or trying to open the gum?
Do not treat it like “regrowth” by trying to remove or scrape tissue. If a tooth is erupting behind gum tissue or a partially erupted wisdom tooth is trapping food, the right step is cleaning the area gently and having a dentist check for impaction or infection rather than attempting home procedures.
Why might one tooth come in much later than others, and is that always a problem?
It’s common for eruption to be slower in some teeth, especially wisdom teeth, but true absence by expected windows can also happen when space is limited or the tooth is angled. A dentist will use the child’s or adult’s age, which tooth it is, and X-ray findings to decide whether monitoring is enough or treatment is needed.
If an impacted tooth is found, how do dentists decide between monitoring and intervention?
Yes, but it’s not guaranteed. When a tooth is impacted or blocked, the outcome depends on the angulation, available space, and root development. Dentists often repeat imaging after a set interval (like 6 to 12 months) to confirm progression before committing to surgical exposure or removal.
Does dental crowding always lead to teeth erupting incorrectly or getting impacted?
Tooth eruption timing and crowding are connected, but crowding alone does not always mean impaction. The pattern of root spacing, jaw size, and tooth angulation matter, so the best way to judge is with appropriate imaging (often panoramic X-rays in adults).
Learn why teeth grow crooked and what causes misalignment, plus practical steps and treatments to fix it
Teeth growth timeline from baby to adult, what can regrow after loss, and realistic options to replace damaged teeth.

Why humans have only baby and permanent teeth: eruption timeline, limits of enamel regrowth, and common exceptions to kn

