No, wisdom teeth do not grow back after they have been properly extracted. Once a tooth is fully removed, the dental tissue that formed it is gone, and your body has no biological mechanism to regenerate an entirely new tooth in its place. That is the short answer. But the longer answer matters, because plenty of people have sworn they felt something growing back after their wisdom teeth were pulled, and in some cases, something really is happening back there. It is just not what they think.
Will Wisdom Teeth Grow Back? After Removal Explained
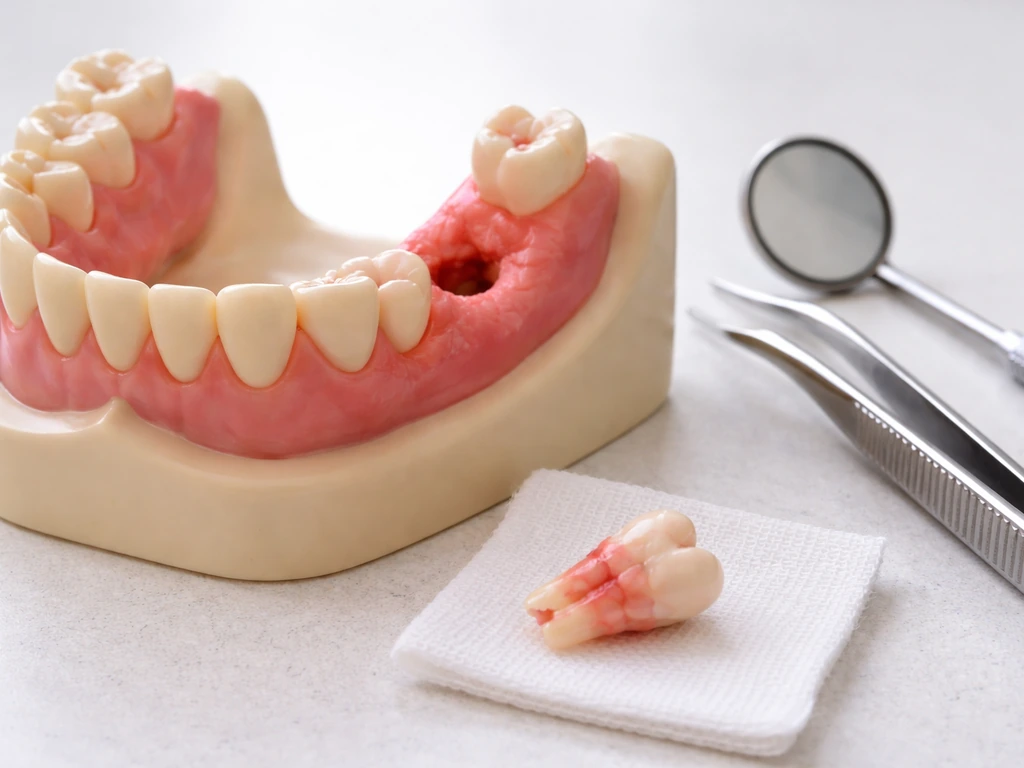
Do wisdom teeth ever grow back after extraction?
The honest answer is no, not in the way most people mean it. True tooth regeneration, where a fully removed tooth simply rebuilds itself from scratch, does not happen in adult humans. We are not sharks. We get two sets of teeth in a lifetime: baby teeth and permanent teeth. Wisdom teeth are part of that second set. Once they are out, they are out for good.
This is not just dental common knowledge, it is basic biology. Human teeth form from a structure called a tooth bud (or dental follicle) during development. Once that bud has formed a tooth and the tooth has been extracted, there is no reserve bud waiting in the wings to produce a replacement. The regenerative machinery simply is not there. So if you had all four wisdom teeth cleanly extracted as an adult and you are now feeling something in the back of your mouth years later, the explanation is not that a new wisdom tooth sprouted. Something else is going on.
Why people think they grew back (what actually changes after removal)
This is probably the most practical part of this article, because the confusion is genuinely common and completely understandable. Here is what people are actually experiencing when they think a wisdom tooth grew back.
Gum tissue heals and changes shape
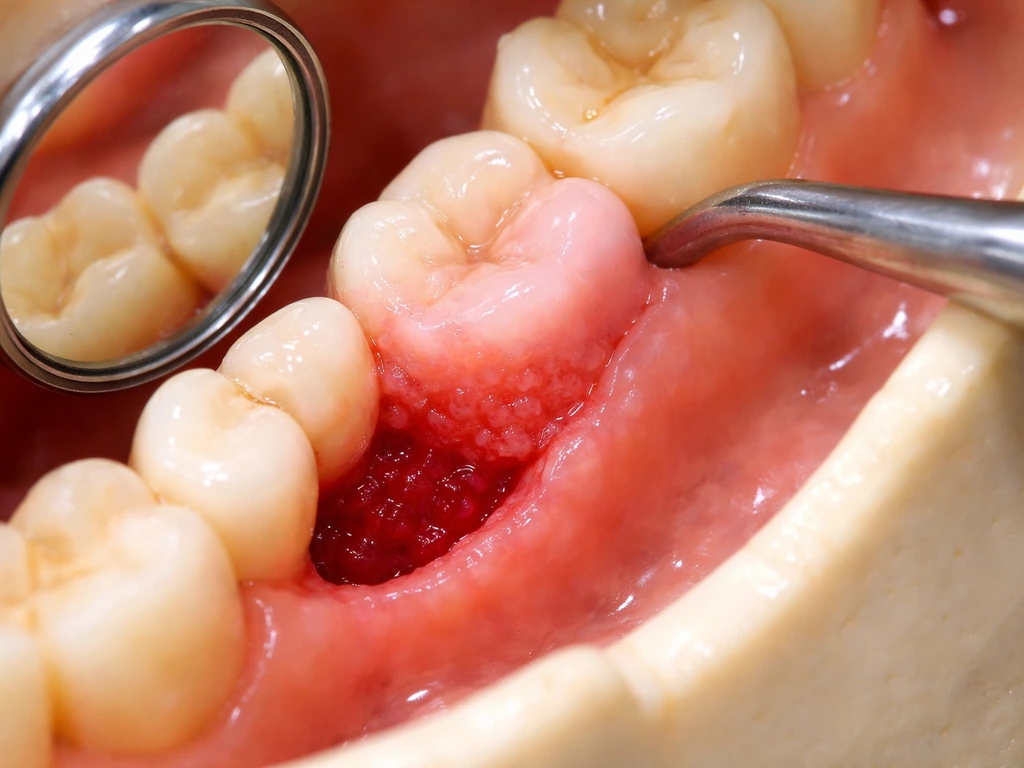
After an extraction, the socket fills in with a blood clot, then granulation tissue, and eventually new bone and gum tissue. That healing process can make the area feel different, lumpy, or raised for weeks to months afterward. Some people notice a firm ridge or bump where the tooth used to be and assume something is growing. It is usually just normal healing, and it typically smooths out over time.
Incomplete extraction left tissue behind
This is the most clinically significant reason. If a root tip, fragment of the crown, or pieces of the dental follicle were left in the socket during extraction, that retained tissue can cause symptoms that feel like a new tooth emerging. A retained root tip, in particular, can work its way toward the surface over time or become a focus of infection and swelling. It is not a new tooth growing, but it can absolutely feel like one.
A different wisdom tooth was still impacted and is now erupting
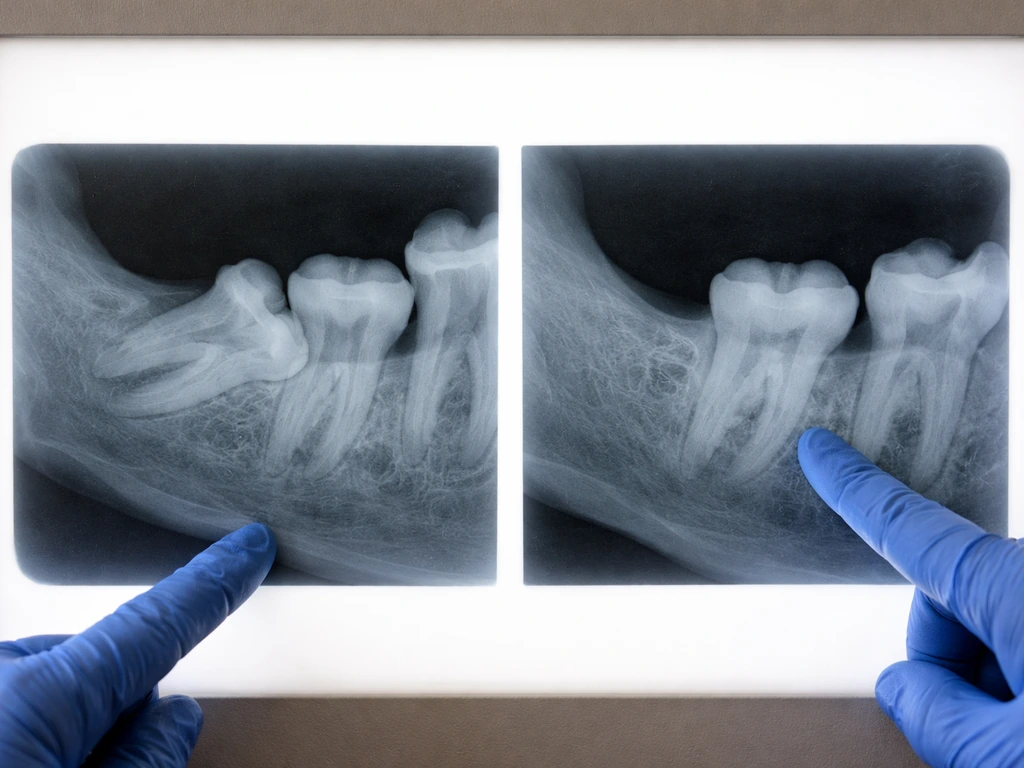
Some people have only one or two wisdom teeth removed, while others remain impacted (stuck under the gum or bone) and were not touched. Months or years later, one of those untreated teeth starts pushing through, and the person connects it to the extraction. This is not regrowth; it is just a separate tooth doing what it was already going to do on its own timeline.
Supernumerary (extra) teeth
Rarely, a person can develop a supernumerary tooth, an extra tooth beyond the standard 32. These are uncommon, but they do exist. If one develops in the wisdom tooth region, it can look like a regrown wisdom tooth. It is not a regenerated tooth; it is an additional developmental anomaly. Your dentist can tell the difference with an X-ray.
Normal eruption timeline vs "regrowth": can new third molars form?
Understanding the eruption timeline helps explain a lot of the confusion here. Wisdom teeth, which dentists call third molars, typically begin erupting between ages 17 and 25. But that range is not rigid. Research tracking third molar eruption from ages 20 to 26 shows that a meaningful proportion of third molars erupt on the later end of that window, meaning some people are still seeing new wisdom tooth activity in their mid-20s.
So here is a scenario that plays out often: a teenager has one or two wisdom teeth start to come in and gets them removed. At 24 or 25, they feel something new in the back of their mouth. They assume their wisdom tooth grew back. Wisdom teeth do hurt for some people as they erupt, so persistent pain is something to evaluate rather than assume it is normal <a data-article-id="8E5A2914-FB06-4D90-9299-CE2DA8167770">do wisdom teeth hurt when they grow in</a>. What actually happened is that another wisdom tooth, which was never removed and was sitting quietly in the jaw, has finally decided to erupt. how long does wisdom tooth take to grow The eruption is right on schedule developmentally; it just feels like a surprise because they thought they were done.
This is why it matters to know exactly how many wisdom teeth you had and how many were extracted. Not everyone has four. Some people have one or two. If you only had two removed and you are now feeling something on the other side, that is eruption of an existing tooth, not regeneration of a removed one.
Rare exceptions and incomplete extraction scenarios
There are a few legitimate exceptions worth knowing about, because they represent real clinical situations where something unexpected can develop in the wisdom tooth area after extraction.
- Retained root fragments: A small piece of root is left behind, either intentionally (when the root is near a nerve) or unintentionally. Over time, this fragment can migrate toward the gum surface, cause discomfort, become infected, or even partially erupt. It requires a follow-up procedure to remove.
- Residual dental follicle tissue: The sac of tissue surrounding a wisdom tooth (the dental follicle) can sometimes be left behind during extraction. In very rare cases, particularly in younger patients whose teeth were still forming, residual follicular tissue could theoretically contribute to further development. This is exceptionally uncommon in fully formed adult teeth.
- Partially impacted tooth never fully extracted: If a deeply impacted wisdom tooth was only partially removed (for example, only the visible portion was extracted and a deeply buried portion was intentionally left), the remaining part may cause ongoing symptoms.
- Misdiagnosis: Sometimes what was thought to be a wisdom tooth on a basic X-ray turned out to be a different structure, and the actual wisdom tooth was never removed at all. This is one reason why advanced imaging is important for accurate diagnosis.
None of these scenarios represent true tooth regeneration. They are all cases where original tissue was present from the start and was either missed, left intentionally, or is continuing its developmental path. The takeaway: if you genuinely had a clean, complete extraction confirmed by your oral surgeon, nothing is growing back from nothing.
How to confirm what's happening today (symptoms + X-rays/CBCT)
If you are feeling something new in the back of your jaw, here is how to figure out what is actually going on. Start by taking stock of your symptoms.
Symptoms worth paying attention to
- A visible or palpable bump or ridge along the gum in the extraction area
- Persistent dull aching or pressure at the back of the jaw
- Pain or discomfort that worsens when chewing or pressing on the area
- Swelling or redness around the original extraction site
- A sensation of something erupting or pushing through the gum
- Difficulty opening your mouth or jaw stiffness on one side
- Bad taste or odor coming from the area (which may suggest infection or a retained fragment)
Mild tenderness and tissue changes within the first few months after extraction are usually part of normal healing. pain when new teeth grow, or that return after the area had fully healed, deserve a proper clinical evaluation. If you want a quick comparison on whether discomfort is tied to normal eruption, see do teeth hurt when they grow in the related guide.
What imaging actually tells you
A standard dental X-ray (periapical or panoramic) is usually the first step. A panoramic radiograph gives your dentist a broad view of all the teeth, the jawbone, and any remaining root tips or bony structures. It is good for a general assessment of what is going on in the wisdom tooth area. However, panoramic X-rays have limits, especially for deeply impacted or complex cases.
For more detailed evaluation, a CBCT scan (cone beam computed tomography) is the gold standard. The American Association of Oral and Maxillofacial Surgeons recommends CBCT in selected cases because it provides three-dimensional imaging of the tooth, roots, surrounding bone, and nearby nerve structures in much greater detail than a flat panoramic image. If there is any uncertainty about retained root tips, residual tissue, or an impacted tooth that was never removed, a CBCT scan will give your oral surgeon a clear, precise picture.
The imaging will not show a regenerated tooth, because there is no such thing to show. What it can reveal is a retained fragment, a previously undetected impacted molar, a supernumerary tooth, or bone and gum changes that explain your symptoms. That clarity is exactly what you need to make a treatment decision.
What to do next: when to see an oral surgeon and likely treatment paths
If you had wisdom teeth removed and are now experiencing new symptoms in that area, here is a practical game plan.
- See your general dentist first. Start with a clinical exam and basic X-ray. Describe exactly when the symptoms started, where they are, and whether they have changed over time.
- Ask specifically about retained root tips or fragments. Tell your dentist you want to rule out any remaining tooth structure from the previous extraction. A periapical X-ray of the specific area is helpful here.
- Request a panoramic X-ray if you have not had one recently. This gives a full view of all remaining teeth and structures, including any impacted molars that may not have been extracted.
- Get a referral to an oral and maxillofacial surgeon if anything is found or if the cause is unclear. Oral surgeons have the training and imaging capabilities (including CBCT) to diagnose and manage complex third-molar situations.
- Ask for a CBCT scan if your surgeon needs better detail. This is especially relevant if there is a suspected impacted tooth near a nerve, or if a retained fragment is in a difficult location.
What treatment typically looks like
| Situation | Likely Finding on Imaging | Typical Treatment |
|---|---|---|
| Pain or bump after extraction, area healed normally | Normal bone remodeling, no retained tissue | Reassurance, monitoring |
| Persistent discomfort with no visible eruption | Retained root tip or fragment | Minor surgical procedure to remove fragment |
| Erupting tissue felt years after removal | Previously impacted tooth now erupting | Evaluation for extraction or monitoring depending on position |
| New eruption on opposite side from extraction | Untouched impacted third molar now erupting | Extraction or monitoring based on position and symptoms |
| Unusual hard tissue in area beyond 32 teeth | Supernumerary tooth | Evaluation, possible extraction if causing problems |
Most of these situations are manageable and straightforward once properly diagnosed. The key is not guessing. An X-ray appointment takes 20 minutes and gives you a definitive answer that no amount of internet research can match.
Can you not grow wisdom teeth at all (agenesis) and what that means after removal
Some people never develop wisdom teeth in the first place. This is called third molar agenesis, and it is surprisingly common. Research puts the prevalence of at least one missing third molar at around 20 percent of the general population. That means roughly one in five people is naturally missing one or more wisdom teeth, with some people having none at all. It is a completely normal developmental variation, not a deficiency.
Agenesis happens because the tooth bud for that particular molar simply never formed during development. If the bud was never there, there was never a tooth to erupt, and there is certainly nothing to grow back after the fact. People who have always been told they do not have wisdom teeth and then feel something new erupting in their late 20s are almost certainly dealing with a very late-erupting third molar that was present but dormant, not a tooth that spontaneously appeared.
If you had wisdom teeth removed and you are wondering whether removal somehow triggers new growth, the answer is definitively no. Extracting a tooth does not stimulate the jaw to produce a replacement in adults. There is no biological feedback loop that says, one tooth was removed, so let us grow another. The developmental process that produces teeth is finished by early adulthood. Removal changes nothing about that.
It is also worth placing this in the broader context of what human teeth can and cannot do. Enamel, the outer protective layer of a tooth, cannot regrow once it is worn or destroyed. Dentin, the layer beneath enamel, has very limited and localized repair capacity through a process involving the pulp, but it does not regenerate the way bone does. Gum tissue can heal after injury, but it does not fully restore to its original architecture without intervention. Wisdom teeth fit into this picture: eruption is a developmental process, not regeneration. A tooth that has fully formed and erupted (or been extracted) has completed its developmental cycle. There is no second act.
The bottom line on wisdom tooth regrowth
<a data-article-id="0101E1DB-3356-4406-B372-681D4DA53C4D">Wisdom teeth do not grow back after extraction</a> What can happen is that retained tissue causes ongoing symptoms, an untouched impacted tooth finally erupts on its own timeline, or healing changes the feel of the extraction site in a way that seems unfamiliar. Wisdom teeth do not grow back after extraction, but if you are trying to understand the timing and location, see where do the wisdom teeth grow as a related reference. how do wisdom teeth grow in. why do wisdom teeth grow sideways
If you are feeling something new in the back of your mouth after a past extraction, the smartest move you can make today is to book an exam with your dentist or oral surgeon and ask for imaging. A panoramic X-ray or CBCT scan will tell you exactly what is there. From that point, you have real information to work with, rather than wondering. And if it turns out nothing concerning is there at all, that is a fast and easy answer worth having.
FAQ
How long after wisdom teeth removal would symptoms from normal healing usually happen?
Normal changes can be noticeable for weeks to a few months, with the most obvious swelling, tenderness, or a firm healing ridge early on. If new symptoms start after the site has felt fully healed, especially recurring pain, increasing swelling, bad taste, or a new hard bump, that points more toward retained tissue, an eruption of an untreated tooth, or inflammation that needs an exam.
If I feel a bump at the extraction site years later, does that automatically mean something was left behind?
Not automatically. A bump can be scar tissue, bone remodeling, or a cystic change, but the key distinction is progression and associated symptoms. A gradually enlarging, painful, or draining area is more concerning than a stable, non-tender ridge, and it warrants imaging to rule out a retained root tip or other cause.
Can an untreated impacted wisdom tooth erupt even after I had the other ones removed?
Yes. If you had one or two removed and the others were left in place, a previously dormant third molar can erupt months or years later. This often feels like “it grew back,” but X-rays usually show a tooth that was never extracted, erupting on its own timeline.
Will a regular dental X-ray always be enough to check for a regrown wisdom tooth?
Often the first step is a panoramic X-ray, but it can miss details in deep or complex areas. If symptoms persist, if the panoramic view is unclear, or if there is concern for retained root tips, an oral surgeon may recommend a CBCT scan because it shows tooth position and nearby structures in 3D.
What symptoms suggest I should not wait and should seek evaluation promptly?
Seek evaluation soon if you have worsening pain, facial swelling, fever, pus or a bad taste/drainage, trouble opening your mouth, numbness or tingling in the lower lip or tongue, or rapid growth of a lump. These can indicate infection, nerve involvement, or a complication that should not be managed by “waiting it out.”
Could it be an infection or cyst rather than a tooth growing back?
Yes. A persistent infection, a dentigerous-type cyst, or inflammation around a retained fragment can create swelling, a firm area, or intermittent pain. Imaging helps determine whether the cause is retained tissue, an adjacent eruption, or another lesion pattern.
How can I tell whether it is a retained root tip versus an eruption of another wisdom tooth?
The most practical differentiator is the pattern on imaging and the timing relative to your original extractions. A retained root tip usually relates directly to the original socket and may show a fragment or bony remnant, while an untreated tooth eruption will show an impacted tooth changing position toward the surface. Your dentist can interpret this once they have the X-ray or CBCT.
Can wisdom teeth grow back if my extraction was only partial or complicated?
If “regrown” is suspected after extraction, it usually means the original process was not a complete removal of all relevant tissue, such as a missed fragment or a residual root tip. Complicated cases can also have slower, uneven healing that feels unfamiliar. A post-extraction scan is the fastest way to confirm what tissue remains.
I was told I have no wisdom teeth, but I feel something erupt in my late 20s. How is that possible?
There are two common explanations: a very late-erupting third molar that was present but never noticed, or a miscommunication from an earlier assessment. True third-molar agenesis means the tooth bud never formed, so there is nothing to erupt, but sometimes earlier imaging did not clearly show the area, or the tooth was simply positioned to be difficult to detect.
If imaging shows nothing concerning, what should I do about lingering soreness or a hard ridge?
Ask whether the discomfort fits normal scar tissue and bone remodeling, and whether any issues like gum inflammation or bite pressure could be contributing. You can also ask about follow-up timing, since some healing changes stabilize over months, but persistent or worsening symptoms should still be rechecked.
Do wisdom teeth “regrow” differently if I get them removed during my teens versus as an adult?
The basic biology does not change. In both cases, a fully extracted, fully formed tooth does not regenerate from a dormant template. The difference is mainly eruption timing, since some people removed wisdom teeth early might later notice activity from a tooth that was never extracted or a tooth erupting on a later schedule.
Learn how long wisdom teeth take to erupt, what delays growth, and when to see a dentist for impaction or pain.
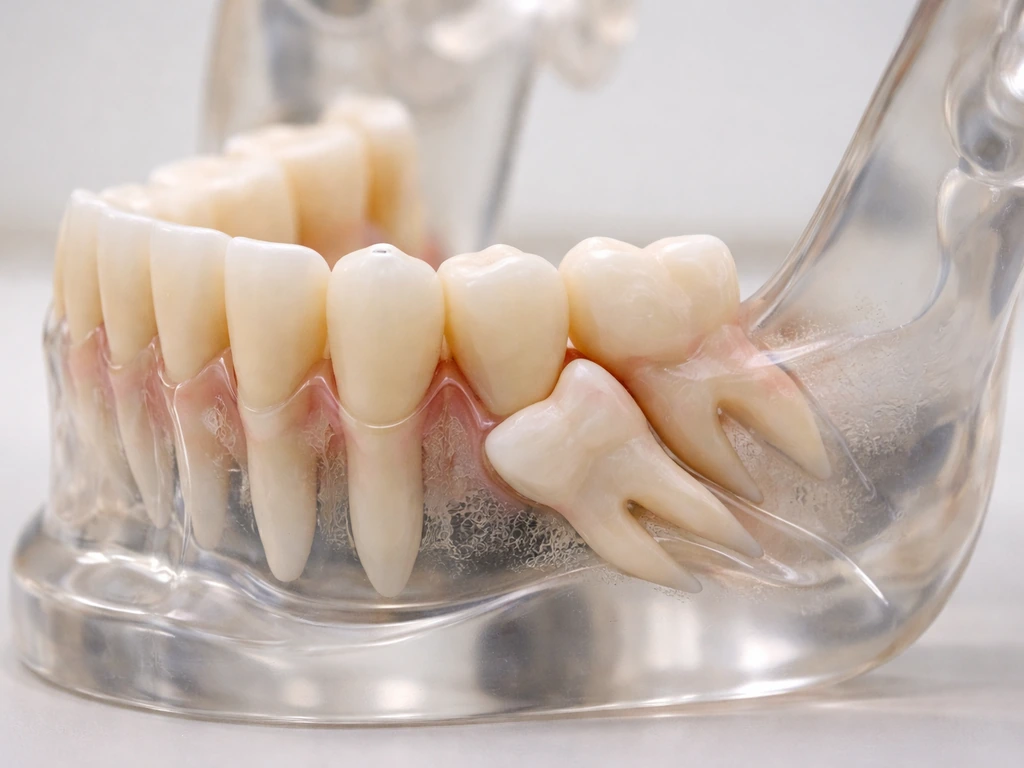
Learn why wisdom teeth grow sideways, what complications to expect, and next steps like X-rays, monitoring, or extractio
Learn where wisdom teeth grow, typical ages, eruption signs, and what to do for pain, impaction, or missing teeth.

