Wisdom teeth grow sideways because there simply is not enough room for them to come in straight. That is the short answer, and it is true for the vast majority of people dealing with this problem. Your jaw did not finish developing with enough space to accommodate a third set of molars erupting at the back, so the tooth tilts, angles, or lies almost completely horizontal as it tries to push through. It is not a personal anomaly or a sign something went seriously wrong with your dental development. It is, in fact, one of the most common dental situations in young adults. how do wisdom teeth grow in
Why Do Wisdom Teeth Grow Sideways? Causes and What to Do
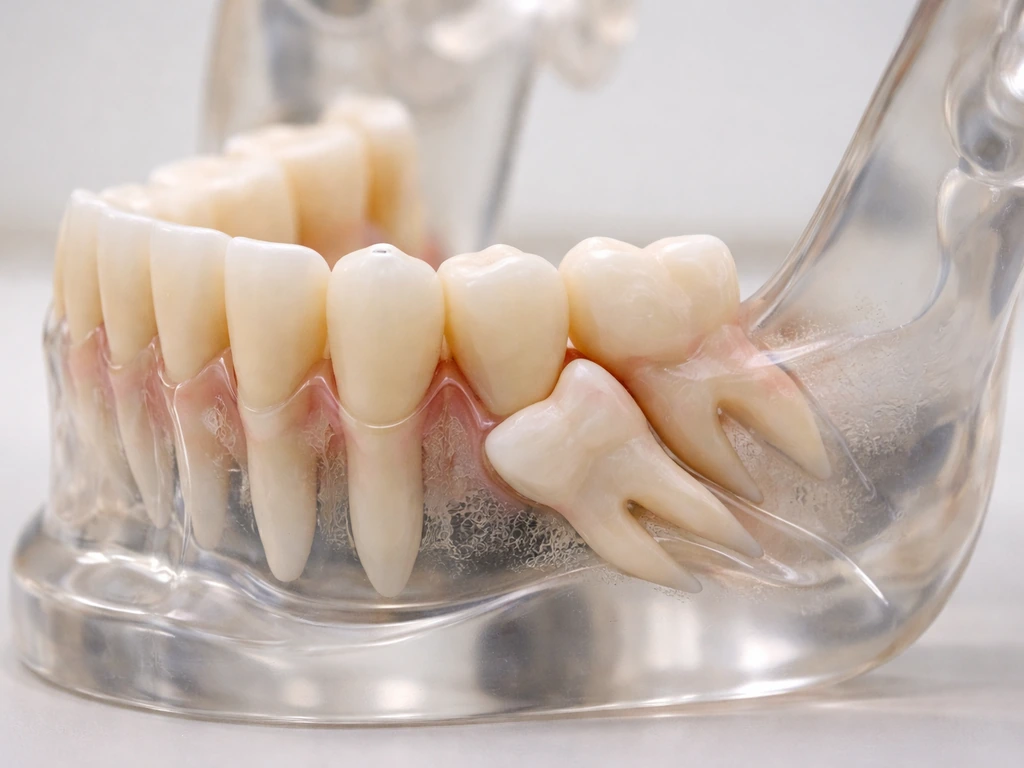
Yes, sideways wisdom teeth are surprisingly common
Here is the first thing to understand: crooked or sideways wisdom teeth are not rare. Research suggests that around 80 out of 100 young adults have at least one wisdom tooth that fails to fully erupt into the mouth. Many of those are partially erupted, impacted at an angle, or lying horizontally in the jaw. One imaging study reported that roughly 24% of impacted lower wisdom teeth were in a horizontal position. So if you are looking at your X-ray thinking something looks wildly wrong, you are actually in a very crowded (pun intended) club.
What people often get wrong is assuming that a sideways wisdom tooth will eventually right itself, or that the gum tissue and jaw will somehow accommodate it over time. That is not how it works. A tooth's eruption path is set by the time it starts moving. If the angulation is off and there is no space, it will not self-correct. There is no biological mechanism for a misaligned wisdom tooth to regenerate into a new position, any more than enamel can grow back after it is lost. Management means monitoring or intervening, not waiting for your body to fix the geometry.
Why wisdom teeth grow sideways: the real causes
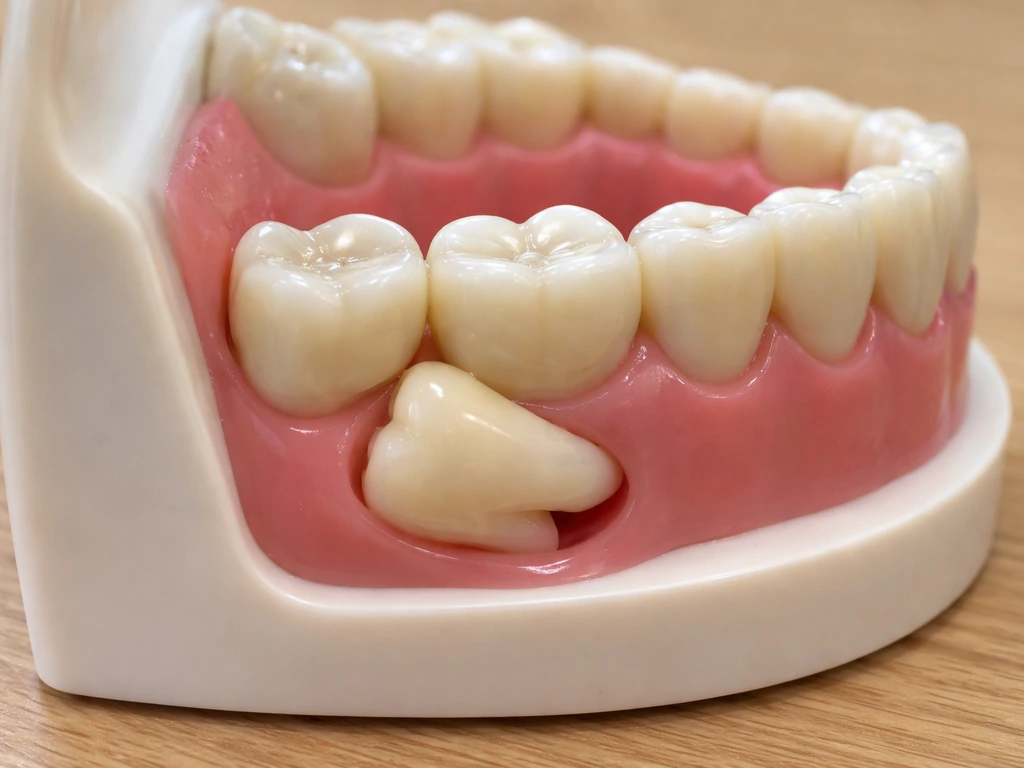
The core reason is a mismatch between tooth size and jaw space. Human jaws have been getting shorter over evolutionary time, but our tooth count has not changed to match. By the time your wisdom teeth start erupting, typically between ages 17 and 25, the back of your jaw is already packed with second molars. There is simply nowhere for the third molar to go in a straight line, so it angles toward whatever path offers the least resistance.
Not enough room in the jaw
This is the number one cause. Impaction happens when complete eruption is blocked by a lack of space, obstruction from an adjacent tooth, or abnormal developmental positioning. The second molar sitting right in front essentially acts as a wall. The wisdom tooth tilts mesially (toward the front of the mouth) to push against it, which is called mesioangular impaction, or it may go almost fully sideways into a horizontal impaction. Some teeth tip backward (distoangular) or come in at an inward or outward angle instead.
Jaw size and genetics

Your jaw dimensions are largely inherited. If your parents had impacted wisdom teeth, there is a reasonable chance you will too. People with smaller jaws, or jaws that did not develop as much arch length as their tooth sizes require, are more prone to third-molar crowding. This is also why some people with wider jaws have their wisdom teeth come in perfectly straight while others in the same family struggle with severe impaction.
Late eruption timing
Wisdom teeth erupt much later than every other permanent tooth, and by the time they start moving, the jaw has already finished growing. Earlier teeth had the advantage of a jaw that was still developing around them. Wisdom teeth do not get that luxury. If the eruption path is blocked, the tooth has no developmental window left to find a clearer route. Late eruption also means the bone around the tooth has become denser, which makes any movement even more restricted.
Tooth angulation and abnormal position during development
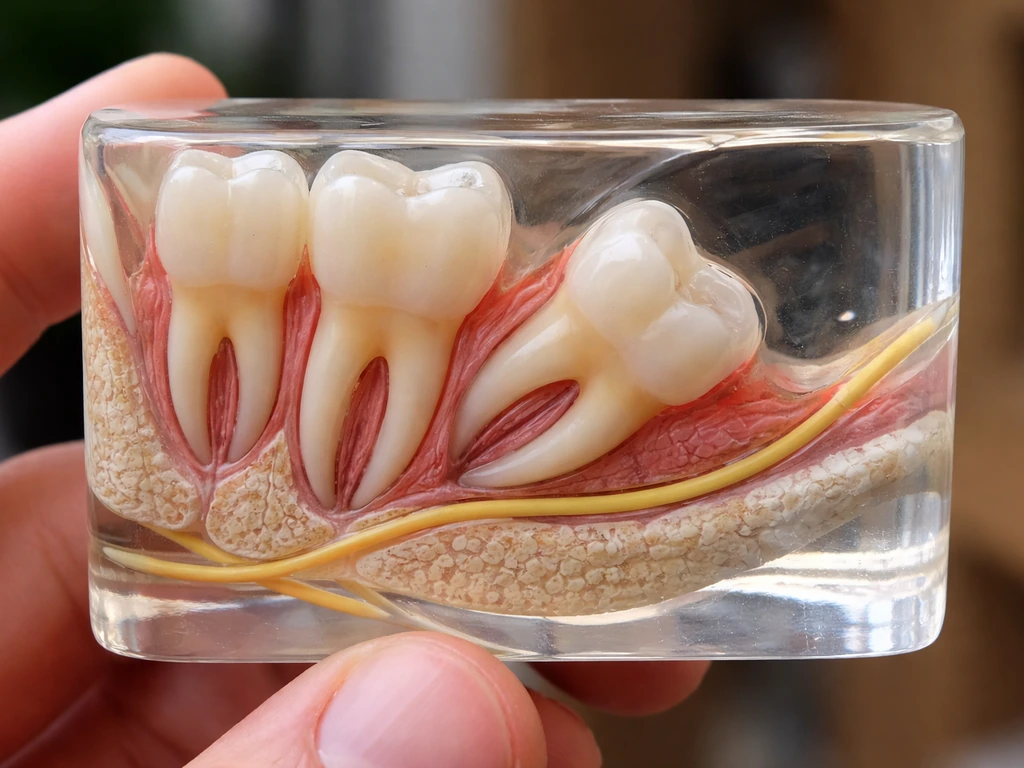
Sometimes the problem starts before the tooth even begins erupting. The third molar can develop at an angle within the jaw, meaning its long axis is already tilted relative to the second molar before any movement begins. Once it starts pushing outward, it follows that built-in angle. Clinicians use classification systems like Winter's classification (which describes the angle of the wisdom tooth relative to the adjacent second molar) and the Pell and Gregory classification (which assesses depth and relationship to the jawbone's ramus) to categorize exactly what kind of impaction is happening.
What happens when a wisdom tooth comes in sideways
A sideways wisdom tooth that is not causing any problems right now might still cause problems later. And if it is already causing symptoms, those can escalate quickly if left alone. Here is what you are actually dealing with when a wisdom tooth erupts at the wrong angle, and whether <a data-article-id="B4E5F709-4500-41A1-87B5-858855538FC0">do wisdom teeth hurt when they grow in</a>:
- Pain and pressure in the back of the jaw, sometimes radiating to the ear, temple, or throat
- Swelling and tenderness in the gum tissue around the partially erupted tooth
- Pericoronitis: infection and inflammation of the gum flap (operculum) that sits over a partially erupted wisdom tooth, collecting bacteria and food debris underneath it
- Difficulty opening your mouth fully (trismus) if swelling becomes severe
- Damage to the neighboring second molar, including root resorption or cavities forming at the contact point between the two teeth
- Increased risk of gum disease and decay on adjacent teeth, which research has confirmed is notably higher with horizontal and mesioangular impaction patterns
- Cyst formation around the crown of an impacted wisdom tooth (called a dentigerous cyst), which can gradually damage surrounding bone
- Chronic partial eruption where the tooth never fully comes in, leaving a permanent gum flap that is difficult to keep clean
Pericoronitis deserves particular attention because it is one of the most common and most uncomfortable complications of sideways wisdom teeth. The partially erupted tooth leaves a pocket of gum tissue that acts like a trap for bacteria. If you are wondering do wisdom teeth hurt when they grow in, that question is closely tied to how a sideways or impacted wisdom tooth erupts and whether symptoms develop. The infection typically starts as localized pain and swelling at the back of the lower jaw, but it can radiate outward as it worsens. If you want to understand what that pain typically feels like and why it happens, see our guide on why does my head hurt when my wisdom teeth grow. In serious cases it progresses to spread beyond the local area, causing fever, difficulty swallowing, or restricted mouth opening. That level of progression is a dental emergency, not something to manage with saltwater at home.
How to tell if your wisdom tooth is actually misaligned
You cannot fully assess the situation yourself, but you can get a reasonable read on what is happening before you see a dentist. Wisdom teeth go through recognizable stages before they become visible: the tooth forms under the gum, then begins to move, then may partially break through the gum (partial eruption), and either continues to full eruption or stalls. If you feel pressure and some soreness at the very back of your mouth but cannot see the tooth yet, it is likely still under the gum. If you can see a white edge or the corner of a tooth peeking through, that is partial eruption.
Symptoms that suggest an abnormal eruption path include persistent pressure against your second molar, pain that is directional (feels like something is pushing from behind), and the visible tooth appearing to lean forward rather than sitting upright. However, the only way to confirm the angulation and depth is with an X-ray. A standard panoramic dental X-ray gives a broad view of all four wisdom teeth and their positions relative to the adjacent molars and jaw structures. For more complex cases, particularly where a lower wisdom tooth appears close to the inferior alveolar nerve (the nerve running through the lower jaw), a cone beam CT (CBCT) scan provides three-dimensional detail that a flat panoramic image cannot fully show.
Clinicians use these images alongside classifications like Pell and Gregory (measuring depth and ramus relationship) and Winter's classification (angulation) to determine how impacted the tooth is and what the risk profile looks like. This is also when the decision about monitoring versus extraction gets its factual grounding. If you have not had a panoramic X-ray taken in the last year or two and you are in your late teens or twenties, getting one is the single most useful thing you can do to understand what is actually happening back there.
What you can do right now while you wait for your appointment

If your wisdom tooth is currently causing discomfort and you are waiting on a dental appointment, there are safe, evidence-supported steps you can take at home. These will not fix the underlying problem, and they will not change the angle your tooth is erupting at, but they can meaningfully reduce pain when new teeth grow and reduce the risk of infection getting worse in the short term.
- Rinse with warm salt water several times a day, especially after meals. This is a recommended first-line management step for localized pericoronitis and helps flush debris from around the gum flap.
- Take over-the-counter pain relief like ibuprofen (if you can tolerate it and have no contraindications), which addresses both pain and inflammation simultaneously.
- Keep the area as clean as possible. Carefully brush around the erupting tooth and use a water flosser or interdental brush if a standard floss cannot reach.
- Avoid very hard, crunchy, or sticky foods on that side of your mouth to minimize irritation to the gum tissue.
- Apply a cold pack to the outside of your jaw for short intervals if swelling is noticeable.
Know when to skip the home remedies and go straight to urgent care. If you develop a fever above 100.4°F (38°C), have trouble swallowing or opening your mouth, experience swelling spreading below your jaw or toward your neck, or have pain that is severe and not responding to over-the-counter medication, those are signs of a spreading infection that needs same-day professional attention. A spreading dental infection can become a serious medical situation quickly, and it is not something to wait out at home.
Your real treatment options and what to expect
Once you have a diagnosis, treatment falls into a few practical categories. Which one is right for you depends on your symptoms, the degree of impaction, whether there is any pathology already present, and your age (younger patients generally have easier extractions because the roots are not fully formed and the bone is less dense).
| Option | When it applies | What it involves | Key consideration |
|---|---|---|---|
| Watchful waiting / monitoring | Tooth is impacted but causing no symptoms and no pathology is present | Regular dental check-ups and periodic X-rays to track any changes | Current guidance (including NICE) does not recommend removing symptom-free, pathology-free impacted wisdom teeth; the evidence for prophylactic removal is limited |
| Extraction by a general dentist | Partially erupted or moderately impacted tooth with manageable position | Local anesthetic, possible small incision in the gum, removal of tooth with or without sectioning it into pieces | Recovery typically 1 to 2 weeks; 3 to 5 days off recommended for impacted cases |
| Oral surgeon referral | Deeply impacted tooth, close proximity to the inferior alveolar nerve, complex anatomy, or failed general dentist removal | Same procedure but with specialist skill and equipment; CBCT imaging often used pre-operatively | Nerve proximity is the key risk factor; paresthesia (temporary or rarely permanent numbness) is a documented complication |
| Management of pericoronitis first, then reassess | Active infection present before any surgical decision | Irrigation, antibiotics if spreading infection, warm salt-water rinses; surgery scheduled after acute phase resolves | Operating through active infection increases complication risk; stabilize first when possible |
The most commonly cited complications from wisdom tooth extraction include dry socket (where the blood clot protecting the healing socket is lost, causing significant pain), post-operative infection, and in a small minority of lower molar extractions, temporary nerve effects. Dry socket rates in clinical reviews have been reported up to around 11%, and lingual nerve or TMJ-related issues each appear in under 1% of cases in reported data. These numbers sound scary in isolation, but for most straightforward extractions the recovery is genuinely manageable. The vast majority of people take a few days off, use prescribed pain relief, and are back to normal within two weeks.
One thing worth being clear about: extraction is the end of the story for that tooth. There is no regeneration. Once a wisdom tooth is removed, it does not grow back. If you have seen articles or social media claims suggesting otherwise, they do not apply to humans. For anyone curious about the broader science of tooth regrowth, that topic is covered separately on this site, but for wisdom teeth specifically: removal is permanent.
Can you prevent wisdom teeth from growing in sideways?
Honestly, not in any reliable way once your jaw has finished developing. The eruption direction is largely determined by your jaw's anatomy and how the tooth's root and crown developed within the bone. You cannot redirect a wisdom tooth's growth path through diet, oral hygiene habits, or any non-surgical intervention. What you can control is how early you catch the problem and how quickly you act when symptoms appear.
Early evaluation makes a real difference. Getting a panoramic X-ray in your mid to late teens lets a dentist or orthodontist see how the wisdom teeth are developing before they start moving in earnest. If crowding or abnormal angulation is visible early, you have more options and easier surgical conditions if extraction becomes the recommended path. Younger patients (late teens to early twenties) tend to have less fully developed roots and softer surrounding bone, both of which make extraction less complicated and recovery faster.
Some orthodontic literature suggests that creating more arch space through orthodontic treatment might theoretically reduce impaction risk, but the evidence that this reliably changes wisdom tooth eruption outcomes is not strong. If you already had orthodontic work done, you may have noticed your orthodontist tracking your wisdom teeth toward the end of treatment. That is standard practice precisely because impacted third molars can put pressure on teeth that were just straightened, though the evidence on how much wisdom teeth actually cause crowding of other teeth is genuinely mixed.
The bottom line on prevention is this: you cannot guarantee your wisdom teeth will come in straight, but you can make sure you have current imaging, see a dentist regularly through your late teens and twenties, and do not ignore new pain or swelling at the back of your mouth. Catching an impaction early, before pericoronitis or damage to the second molar has set in, puts you in a much better position for whatever management comes next.
FAQ
Can my wisdom tooth grow sideways and still come in normally later?
In most cases, no. Once the tooth has started erupting along an angled path with no space, it generally does not realign itself. It may continue partial eruption or remain impacted, and the longer it sits half-covered, the higher the chance of recurring gum inflammation.
What’s the difference between a sideways wisdom tooth and one that is just “partially erupted”?
A partially erupted tooth can be angled, but it can also be fairly upright while only breaking through partway. Sideways implies the tooth’s long axis is tilted relative to the second molar, which can increase the risk of trapped food debris, pericoronitis, and pressure on the adjacent tooth.
If I don’t have pain right now, should I still get an X-ray?
Yes, especially if you are in your late teens to mid twenties or you have a family history of impacted third molars. Symptoms can show up later, but the decision to monitor versus extract is easier to make when you know the tooth depth and angulation from imaging.
How often should someone with impacted or erupting wisdom teeth be monitored?
A common approach is re-checking at set intervals (often every 6 to 12 months) when the tooth is not immediately causing problems. The exact schedule depends on risk factors like recurrent gum swelling, proximity to nearby roots or nerves, and whether there is decay or gum disease around the second molar.
Can poor oral hygiene be the cause of a sideways eruption?
Oral hygiene usually affects infection and gum health, not eruption direction. It can worsen pericoronitis because bacteria and food collect around a partially erupted flap, but it does not create the lack of space or the angled tooth position that drives impaction.
Is it safe to try home remedies like salt water or clove oil while waiting for care?
Salt water rinses can be reasonable for comfort, they do not correct impaction. Avoid numbing gels or strong remedies that mask worsening symptoms, and do not rely on them if you develop fever, spreading swelling, trouble swallowing, or worsening jaw tightness.
Why does pericoronitis keep coming back if I’ve already treated the episode once?
Because the underlying geometry often stays the same, the gum flap can continue to trap bacteria and food. If episodes recur, clinicians may recommend definitive treatment such as extraction rather than repeated temporary symptom control.
What imaging is best, panoramic X-ray or CBCT?
A panoramic X-ray is usually the first step because it shows the positions of all wisdom teeth relative to surrounding structures. CBCT is more likely when a lower tooth appears close to the nerve canal, when anatomy looks complex, or when the clinician needs three-dimensional detail for surgical planning.
Does a wisdom tooth growing sideways damage my other teeth?
It can. Impacted teeth can place chronic pressure on the second molar, contribute to gum pocketing and inflammation, and increase the risk of decay in the area around the contact point. This is one reason monitoring is not always “do nothing.”
Is extraction harder in older patients, and what changes with age?
Often, yes. With age, roots tend to be more developed and surrounding bone can be denser, which can make surgery more technically demanding and recovery slower. That said, the specific difficulty depends on angulation, depth, and proximity to nearby structures, not age alone.
How do I know whether I’m dealing with an eruption under the gum versus an already visible tooth?
Pressure or soreness at the back of the mouth without a visible tooth often suggests the tooth is still covered or only beginning to emerge. Seeing a corner or white edge usually indicates partial eruption. However, the definitive assessment still requires imaging because symptoms can overlap with infection.
Can orthodontic treatment prevent sideways wisdom teeth?
Orthodontics may help with arch space and alignment, but the evidence that it reliably changes wisdom tooth eruption outcomes is not strong. Your orthodontist might still track them near the end of treatment because impacted third molars can influence nearby teeth, especially if space is tight.
If I remove the wisdom tooth, will I ever need to worry about it coming back?
No. For humans, extraction is permanent for that tooth. The tooth cannot regrow or redirect because the tooth-forming tissue does not regenerate into a new erupted replacement.
Learn where wisdom teeth grow, typical ages, eruption signs, and what to do for pain, impaction, or missing teeth.
How wisdom teeth grow in: timing, proper eruption, common misgrowth, myths, and when to get X-rays or urgent care.

Understand if teeth hurt as they erupt, what’s normal vs damage, and get safe relief plus red-flag when to see a dentist

