Wisdom teeth grow at the very back of your mouth, one in each corner of your jaw. There are up to four of them total: two on the top (upper arch) and two on the bottom (lower arch), each sitting directly behind your second molars. They are your third molars, and they are the last permanent teeth to arrive. If you are feeling pressure, soreness, or something pushing through your gums way at the back, that is almost certainly what is happening. If you are wondering whether do wisdom teeth hurt when they grow in, that gum flap and early pressure are often the reason you feel soreness before the tooth is fully through. why does my head hurt when my wisdom teeth grow
Where Do Wisdom Teeth Grow: Timing, Signs, and What to Do
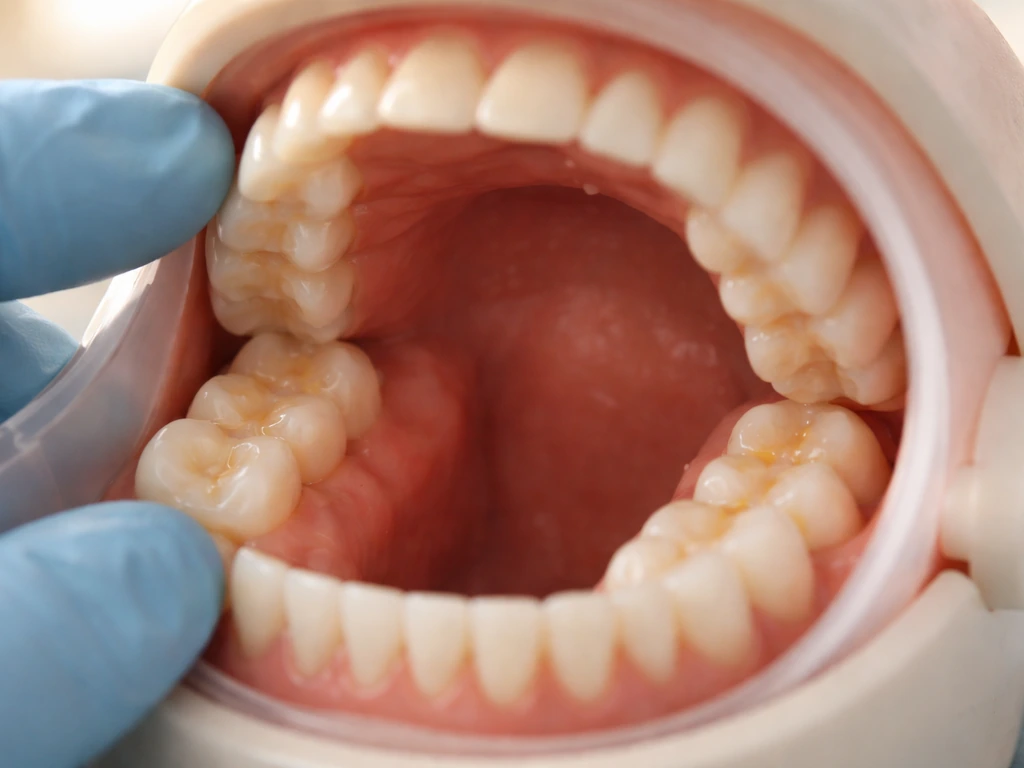
Exactly where in the mouth wisdom teeth grow
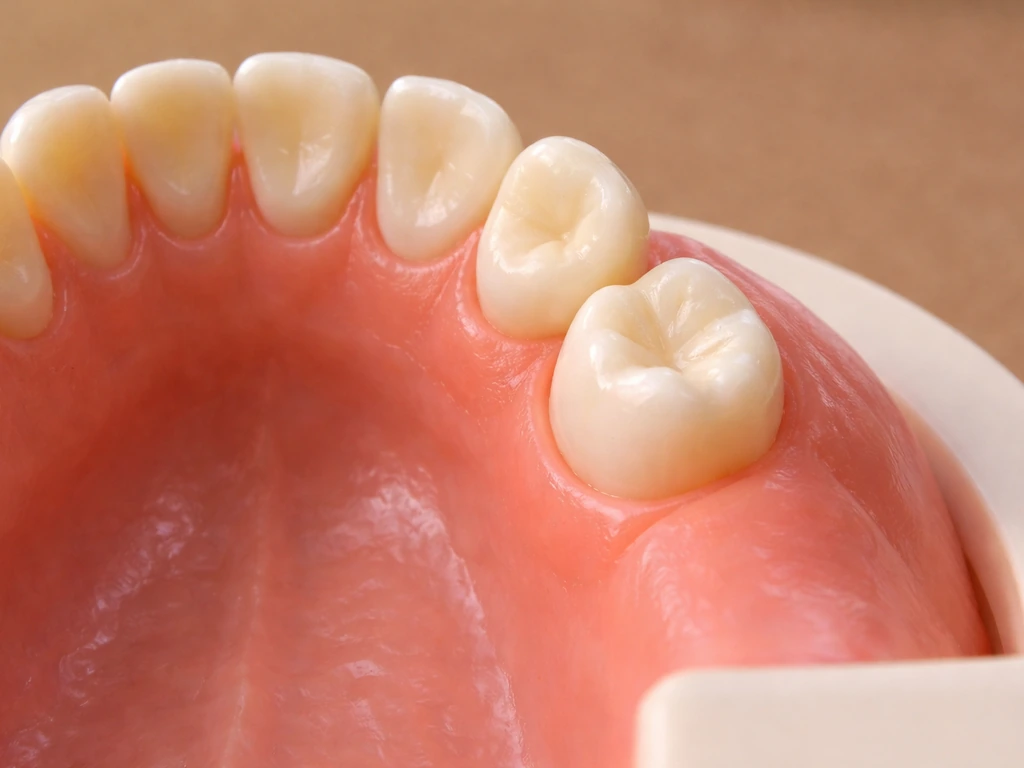
Each wisdom tooth erupts at the far posterior end of its dental arch. The upper ones push through the gum behind your upper second molars (the maxillary third molars), and the lower ones do the same behind your lower second molars (the mandibular third molars). In a full adult set of 32 teeth, wisdom teeth occupy positions 1, 16, 17, and 32, the four outermost corners of the mouth.
Because they erupt so far back, wisdom teeth have very little room to work with. The jawbone and the existing second molars are right there, and the gum tissue forms a small flap over the emerging crown. That flap is actually the source of a lot of wisdom tooth pain, more on that shortly. The location is also why you can feel pressure deep in your jaw rather than pain on an obvious visible tooth, especially early on when the crown is still under the gum surface.
When wisdom teeth actually erupt: a timeline by age
The classic answer is ages 17 to 25, and that is accurate for most people. But the timeline is not a single event, it has distinct phases, and understanding them helps you know whether what you are experiencing right now is normal or not.
When they start (ages 17–20)
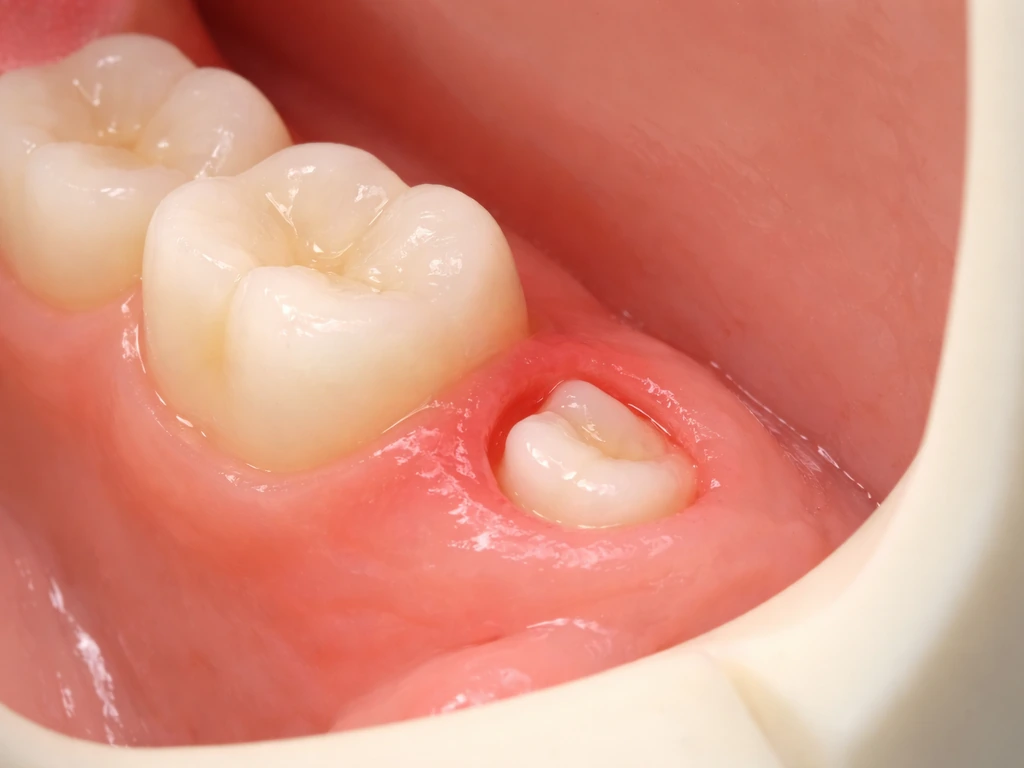
Wisdom teeth typically begin their eruption attempt in the late teens. For many people, the first signs of movement start around age 17 or 18: aching at the back of the jaw, some tenderness in the gum, and if you are getting regular dental X-rays, your dentist will see the crowns beginning to orient toward the surface. This is the phase when impaction problems become visible on imaging, even before you feel anything dramatic.
When they are fully erupted (ages 18–25)
Full eruption, when the crown has completely broken through the gum and the tooth is in its final position, typically happens somewhere between 18 and 25 for most people. Research suggests that third molar eruption is generally completed between ages 17 and 20 in many patients, though some teeth continue to upright and settle into position until around age 25. So if you are 22 and your wisdom teeth are still moving, that is within normal range.
When they "grow out" (mid-20s and beyond)
Some people use the phrase "grow out" to mean the tooth has fully emerged and stabilized, which can happen as late as the mid-20s. Others use it to ask whether wisdom teeth eventually stop causing problems on their own, and the honest answer is: sometimes yes, sometimes no. A tooth that erupts cleanly and has room to sit upright can become a fully functional molar with no issues. One that partially erupts and stays half-covered by gum tissue can cause recurring problems for years. Studies show that pericoronitis (gum inflammation around a partially erupted wisdom tooth) has its highest incidence in patients aged 26 to 35, meaning these teeth can keep causing trouble well into adulthood if left unaddressed.
| Age Range | What's Typically Happening |
|---|---|
| Under 17 | Wisdom teeth are developing below the gumline but have not erupted; usually no symptoms yet |
| 17–20 | Eruption begins; pressure, soreness, and early gum swelling are common |
| 18–25 | Most wisdom teeth reach full or near-full eruption; impaction usually becomes clear by now |
| 25+ | Eruption is largely complete; teeth that are still partially covered can cause ongoing issues |
Does everyone get wisdom teeth? Stages, frequency, and are you born with them?
No, not everyone gets wisdom teeth. Some people develop all four, some develop one or two or three, and some develop none at all. The condition of being born without wisdom teeth is called third molar agenesis, and it is genuinely common. Research on modern populations confirms that congenital absence of third molars exists across all groups, with rates varying by ancestry and individual genetics.
You are not actually "born with" wisdom teeth in the sense that they are present at birth. The way wisdom teeth grow in depends on how and when your third molars develop under the jawbone <a data-article-id="B4E5F709-4500-41A1-87B5-858855538FC0">how do wisdom teeth grow in</a>. Like all permanent teeth, they form gradually under the jawbone during childhood and adolescence, with the crown developing first and the roots continuing to form through the eruption process. By the mid-teens, a dental X-ray can usually show whether wisdom teeth are present and how they are positioned. If they are not visible on imaging by the late teens, a dentist can often confirm whether they are simply absent or just delayed.
As for whether they arrive in stages: yes, it is completely normal for wisdom teeth to erupt at different times. You might get one lower wisdom tooth at 18, have no activity for a year, and then feel a upper one beginning to push through at 20. They do not emerge in a coordinated set, each one follows its own schedule based on its individual position in the bone and the available space in that part of your jaw.
Why wisdom teeth grow at all: the biology behind late eruption
Wisdom teeth exist because humans are designed to grow 32 teeth, and third molars are simply the last set in that biological sequence. Evolutionarily, our ancestors had larger jaws and a diet that wore down teeth significantly, meaning extra molars in the back were useful and had room to erupt without crowding. The problem is that modern human jaw size has trended smaller over generations, while the genetic blueprint for growing third molars has largely stayed the same. The result: a late-erupting tooth that frequently runs out of space.
The trigger for eruption itself is a combination of root development and the resorption of bone along the eruption path. As wisdom tooth roots grow, they generate pressure that drives the crown upward through the bone and gum. When there is not enough space in the dental arch, or when the tooth is angled in an unfavorable direction, this eruption force gets blocked. Dense overlying bone and a compressed arch are the two main physical reasons eruption fails or stalls, resulting in an impacted tooth.
Normal symptoms vs. warning signs when wisdom teeth come in
Some discomfort when wisdom teeth erupt is completely expected. Knowing what is normal versus what needs prompt attention can save you a lot of anxiety, or help you catch a problem before it gets serious.
What is normal
- Mild to moderate aching or pressure at the back of the jaw
- Tenderness and slight swelling in the gum directly over the erupting tooth
- A small amount of redness around the gum flap covering the emerging crown
- Occasional soreness that comes and goes over days or weeks
- A faint salty or metallic taste from minor gum irritation
Much of this soreness is driven by pericoronitis, which is the medical term for inflammation of the gum tissue surrounding a partially erupted wisdom tooth. It is extremely common, especially in the lower jaw. Mild pericoronitis typically causes localized pain and swelling around the back tooth and often resolves once the tooth erupts more fully or is treated.
Warning signs that need prompt attention
- Fever alongside jaw pain or swelling
- Difficulty opening your mouth (this is called trismus and indicates possible spreading infection)
- Severe, worsening pain that is not responding to over-the-counter relief
- Visible swelling that extends beyond the gum into the cheek or throat area
- Unpleasant taste or discharge that does not clear up
- Pain radiating toward the ear or down the jaw
These are signs that a mild pericoronitis has escalated into a more serious infection. Fever and restricted mouth opening, in particular, indicate that infection may be spreading beyond the local gum tissue. This is not a wait-and-see situation. You need to see a dentist or oral surgeon that day.
What happens if you let wisdom teeth grow in, or if they do not
This is where outcomes split into two very different paths, and the direction depends almost entirely on whether the tooth has enough space and the right angle to erupt cleanly.
If a wisdom tooth grows in fully with no problems
If there is adequate room and the tooth comes in upright, it can become a functional molar. You will brush and floss it like any other tooth, and it can last a lifetime. The main challenge is that wisdom teeth are hard to reach, so they require careful cleaning to avoid cavities. If they erupt cleanly and you can maintain them, there is generally no reason to remove them. NICE guidance supports this: impacted wisdom teeth that are not causing problems do not automatically need to come out, but they do need regular monitoring at dental check-ups.
If a wisdom tooth becomes impacted
Impaction means the tooth cannot fully erupt because it lacks space or has an unfavorable angle. Impaction means the tooth cannot fully erupt because it lacks space or has an unfavorable angle. It may push sideways into the adjacent second molar, angle forward (mesioangular impaction), angle backward (distoangular), or lie almost completely horizontal., angle forward (mesioangular impaction), angle backward (distoangular), or lie almost completely horizontal. About 36 to 46 percent of third molars are impacted globally, based on large-scale systematic review data, making this genuinely common, not a rare edge case.
The consequences of leaving a problematic impacted tooth in place are real. Research documents that impacted lower wisdom teeth increase the risk of cavities and gum disease on the back side of the adjacent second molar, and in some positions they can even cause external root resorption of that second molar, meaning the second molar's root is slowly damaged by the pressure. This is one of the stronger arguments for proactive evaluation rather than indefinitely ignoring an impacted tooth.
If wisdom teeth never come in at all
If your wisdom teeth simply did not develop (congenital agenesis), there is nothing to erupt and nothing to worry about. If they developed but are deeply embedded and not erupting, a dentist can monitor them over time with periodic X-rays. Teeth that stay fully enclosed in bone without causing pathology are sometimes left alone, though they still need to be watched for cyst formation around the follicle.
One thing wisdom teeth cannot do: grow back after removal
Once a wisdom tooth is extracted, it {{will not regrow}}. Adult teeth, including third molars, do not regenerate after removal, that is a biological fact, not a dental opinion. There is no known natural mechanism for adult tooth regeneration in humans. If you have had a wisdom tooth removed and feel something in that area again, it is worth getting checked, but it is far more likely to be scar tissue, bone remodeling, or an adjacent tooth shifting than a regenerated molar. If you want to understand more about why permanent teeth cannot grow back, that topic is covered elsewhere on this site.
What to do right now: symptom relief, self-checks, and when to call a dentist
Managing symptoms at home
If you are experiencing mild eruption discomfort and there are no red flags, these steps can help while you arrange a dental visit:
- Rinse gently with warm salt water (half a teaspoon of salt in a glass of warm water) two to three times a day. This reduces bacteria around the gum flap and calms mild inflammation.
- Take an over-the-counter anti-inflammatory like ibuprofen if it is appropriate for you. It addresses both pain and the underlying inflammation more effectively than acetaminophen alone for this type of soreness.
- Keep the area clean. Use a soft-bristled toothbrush and brush as far back as you comfortably can. Food debris trapped under the gum flap is the primary driver of pericoronitis flare-ups.
- Avoid pressing on the area with your tongue or fingers. Repeatedly probing it makes the tissue more irritated.
- Avoid very hard, crunchy foods on that side until the acute tenderness settles.
How to check yourself
Use a flashlight and a mirror to look at the back of your lower jaw, which is where symptoms most commonly start. You are looking for a partially visible tooth crown, a visible gum flap that looks red or puffy, or any discharge. Upper wisdom teeth can be harder to see on your own. If you cannot see clearly but are feeling pressure or pain, do not try to diagnose it yourself. A dental X-ray is the only reliable way to see what is happening beneath the gum.
When to see a dentist, and how urgent it is
| Situation | How Soon to Act |
|---|---|
| Mild soreness, slight gum swelling, no fever | Book a routine appointment within a week or two |
| Recurring pain that keeps coming back every few weeks | See a dentist soon to discuss X-ray evaluation and options |
| Significant swelling, pain worsening over 2–3 days | See a dentist within 24–48 hours |
| Fever, difficulty opening mouth, swelling spreading to cheek/neck | Seek same-day dental or urgent care — do not wait |
At the appointment, your dentist will do a clinical exam and almost certainly take a panoramic X-ray (an OPG) if you do not have a recent one. That X-ray shows all four wisdom teeth at once, their angles, their root development, their proximity to the nerve in the lower jaw, and whether any impaction is present. From there, you will get a clear picture of whether your wisdom teeth can be monitored, whether they need removal, or whether they are already causing damage to adjacent structures.
If your dentist refers you to an oral and maxillofacial surgeon for evaluation, that is routine, not alarming. Surgical extraction of impacted third molars is one of the most commonly performed dental procedures, and an experienced surgeon will walk you through exactly what to expect. The AAOMS recommends evaluation by an oral and maxillofacial surgeon whenever symptoms from impacted wisdom teeth are present. Getting that evaluation done sooner rather than later gives you the most options and helps protect the second molar sitting right next to it.
FAQ
How far back do wisdom teeth grow in your mouth (what teeth do they sit next to)?
They erupt directly behind your second molars, so the “back tooth” that comes in last is your third molar (one in each quadrant, top left, top right, bottom left, bottom right). If you are pointing to a tooth that is already at the very back of your jawline, it is usually not a wisdom tooth unless it is specifically behind the second molar.
Can wisdom teeth grow in if my mouth feels “too small” or my teeth are already crowded?
Yes. Crowding is a risk factor because there is less space for the crown to emerge upright, so the tooth is more likely to stay partially covered by gum or tilt into the second molar. Even if crowding exists, the deciding factor is the tooth’s angle and available space, which an OPG/panoramic X-ray can show clearly.
Why do I feel pain deep in my jaw instead of on a visible tooth?
In the early eruption phase, part of the crown is still under the gum flap, so inflammation (often pericoronitis) can feel like deep pressure rather than a sharp, localized spot. That is one reason a visible “bad tooth” may not appear even though symptoms are real.
Are all four wisdom teeth supposed to come in around the same time?
No. Each third molar can follow its own schedule based on its position and how its roots develop. It is common for one side to start around 18 while another tooth may not attempt eruption until years later, or never erupt at all.
If my wisdom teeth erupt fully, can they still cause problems later?
They can, mainly because the far-back location is harder to clean well. Even when a tooth erupts into position, the gum line around it can trap food and plaque, raising the risk of cavities and gum inflammation on the back side.
What does “partially erupted” mean, and why does it matter?
Partially erupted means a portion of the crown is out of the bone while a gum flap still covers the rest. That flap can collect debris and bacteria, triggering recurring pericoronitis. Once fully erupted and accessible, symptoms are often less likely to keep returning.
When should I stop managing symptoms at home and get urgent care?
Seek same-day evaluation if you have fever, worsening swelling, trouble opening your mouth, rapidly increasing pain, or pus or bad taste/discharge that keeps coming back. Those signs can suggest infection spreading beyond the local gum tissue.
How can I tell whether my pain is from a wisdom tooth versus something else?
The “where” and “when” help, pain that is centered behind the second molar, gum swelling over a half-covered crown, and symptoms that flare with biting or chewing often point to pericoronitis. However, because other issues (cavities, gum disease, tooth cracks, sinus-related pain) can mimic it, a dental exam and usually an X-ray are the reliable way to confirm the source.
Can a dentist confirm on an X-ray whether my wisdom teeth are present or absent?
Yes. A panoramic X-ray (OPG) can show whether third molars are present, delayed, or impacted, and it can also assess angulation and how close the lower roots are to the nerve. If wisdom teeth are not visible by the late teens, imaging can help distinguish absence from delayed eruption.
If an impacted wisdom tooth is not causing symptoms, do I still need monitoring?
Often yes. Some impacted teeth stay quiet, but they can later contribute to gum disease or cavities on the adjacent second molar. Regular dental check-ups with periodic imaging help track position changes or new signs of pathology.
What happens if I have a wisdom tooth extracted, will the space refill?
No. Once a wisdom tooth is removed, the tooth does not regrow. If you notice new pain later in that area, it is more likely scar tissue, normal healing, bone remodeling, or issues with neighboring teeth rather than regeneration.
Does it matter whether the wisdom tooth is upper or lower for risk and symptoms?
Yes. Lower wisdom teeth are more commonly associated with pericoronitis because of the gum flap behavior and the way the lower back area tends to collect debris. Lower impactions also need careful assessment because of proximity to the nerve in the lower jaw.
How wisdom teeth grow in: timing, proper eruption, common misgrowth, myths, and when to get X-rays or urgent care.

Understand if teeth hurt as they erupt, what’s normal vs damage, and get safe relief plus red-flag when to see a dentist
Yes, wisdom teeth can hurt during eruption with pressure, dull ache, gum irritation. Learn relief, timelines, and when t

